-
-
-
Jakarta, Indonesia
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps

Blood Pressure Monitoring as a Public Health Priority: Strengthening Early Detection and Long-Term Cardiovascular Prevention
Blood pressure monitoring is one of the simplest clinical practices in medicine, yet its public health value is profound. Hypertension remains a leading modifiable risk factor for stroke, ischemic heart disease, heart failure, chronic kidney disease, and premature death worldwide. Despite this, a large proportion of individuals with elevated blood pressure remain undiagnosed, undertreated, or inadequately controlled. In this context, blood pressure monitoring should not be viewed merely as a routine measurement performed during clinic visits, but as a central prevention strategy capable of influencing population-level cardiovascular outcomes.
The importance of monitoring begins with the nature of hypertension itself. Elevated blood pressure is frequently asymptomatic, allowing vascular injury to progress silently over years before clinical events occur. Many patients first learn they have hypertension only after presenting with complications such as stroke, myocardial infarction, or kidney dysfunction. This silent progression makes regular measurement essential. Unlike diseases that require complex diagnostic procedures, hypertension can often be detected through accessible and relatively low-cost methods, which makes blood pressure monitoring especially suitable for broad public health implementation.
Traditionally, office-based measurement has been the main foundation of hypertension detection. However, relying only on occasional clinic readings has important limitations. Some individuals exhibit white-coat hypertension, in which blood pressure is elevated in a clinical setting but not in daily life. Others have masked hypertension, where clinic values appear normal despite persistently high blood pressure outside the office. These patterns highlight why modern strategies increasingly emphasize repeated measurement, home blood pressure monitoring, and, when indicated, ambulatory blood pressure monitoring. Together, these approaches provide a more accurate picture of true blood pressure burden and improve clinical decision-making.
Home blood pressure monitoring has gained particular importance in recent years. It supports patient engagement, allows repeated assessment over time, and may help clinicians distinguish persistent hypertension from situational elevation. For patients already diagnosed with hypertension, home monitoring can improve adherence, encourage lifestyle awareness, and provide clearer data for treatment adjustment. From a public health perspective, this approach also supports decentralization of chronic disease management, especially in communities with limited access to frequent in-person care. As digital health tools continue to expand, integration of validated home devices with telemedicine and primary care follow-up may further enhance hypertension control.
Accurate technique remains a critical issue. The value of blood pressure monitoring depends not only on how often it is performed, but also on whether it is done correctly. Inaccurate cuff size, poor body positioning, inadequate rest before measurement, conversation during assessment, and use of nonvalidated devices can all produce misleading readings. For that reason, public health initiatives should not focus solely on increasing the number of measurements, but also on improving the quality of measurement practices. Training healthcare workers, educating patients, and promoting validated devices are all necessary steps in strengthening blood pressure surveillance.
The public health significance of blood pressure monitoring extends beyond diagnosis. It plays a direct role in risk stratification and long-term prevention. Persistent elevation in systolic or diastolic pressure contributes to cumulative vascular injury, endothelial dysfunction, arterial remodeling, and target organ damage. Regular monitoring allows earlier intervention through lifestyle counseling, salt reduction, weight management, physical activity, smoking cessation, and pharmacologic therapy when needed. In this way, blood pressure measurement becomes the gateway to preventing far more costly and disabling outcomes later in life.
Monitoring is also relevant at the population level because hypertension control remains uneven across regions and healthcare systems. In many low- and middle-income countries, awareness, treatment access, and continuity of care remain limited. Even in higher-resource settings, many patients diagnosed with hypertension still do not achieve recommended blood pressure targets. Public health programs that include community screening, workplace checks, pharmacy-based monitoring, and primary care follow-up can help close this gap. Such programs are especially important for high-risk groups, including older adults, individuals with diabetes, patients with obesity, and those with a family history of cardiovascular disease.
Another important dimension is the role of blood pressure monitoring in reframing prevention as an ongoing process rather than a one-time event. A single normal reading does not eliminate future risk, just as one elevated reading does not always confirm chronic hypertension. Longitudinal observation is therefore essential. This perspective is particularly relevant in public health, where continuity and repeated engagement are often more effective than isolated interventions. When monitoring is embedded into regular health behavior, it supports a culture of early detection and long-term self-management.
Scientific evidence consistently shows that improved blood pressure detection and control are associated with meaningful reductions in stroke, coronary events, heart failure, and renal disease. Yet the persistence of poorly controlled hypertension worldwide suggests that monitoring strategies are still underutilized or inconsistently implemented. Public messaging often emphasizes treatment, but monitoring itself deserves greater attention as the first practical step in prevention. Without reliable measurement, there can be no accurate diagnosis, no rational therapy adjustment, and no effective long-term control.
In conclusion, blood pressure monitoring remains a cornerstone of modern public health and cardiovascular prevention. Its value lies not only in identifying hypertension, but also in improving treatment precision, patient engagement, and long-term risk reduction. Expanding access to accurate and repeated blood pressure measurement in clinics, homes, and communities should be considered a strategic priority in efforts to reduce the global burden of cardiovascular and renal disease.
References
1. World Health Organization. Guideline for the pharmacological treatment of hypertension in adults. Geneva: WHO. 2021.
2. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Hypertension. 2018;71(6):e13-e115.
3. Unger T, Borghi C, Charchar F, et al. 2020 International Society of Hypertension Global Hypertension Practice Guidelines. Hypertension. 2020;75(6):1334-1357.
4. Stergiou GS, Palatini P, Parati G, et al. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. Journal of Hypertension. 2021;39(7):1293-1302.
5. Mills KT, Stefanescu A, He J. The global epidemiology of hypertension. Nature Reviews Nephrology. 2020;16(4):223-237.
The importance of monitoring begins with the nature of hypertension itself. Elevated blood pressure is frequently asymptomatic, allowing vascular injury to progress silently over years before clinical events occur. Many patients first learn they have hypertension only after presenting with complications such as stroke, myocardial infarction, or kidney dysfunction. This silent progression makes regular measurement essential. Unlike diseases that require complex diagnostic procedures, hypertension can often be detected through accessible and relatively low-cost methods, which makes blood pressure monitoring especially suitable for broad public health implementation.
Traditionally, office-based measurement has been the main foundation of hypertension detection. However, relying only on occasional clinic readings has important limitations. Some individuals exhibit white-coat hypertension, in which blood pressure is elevated in a clinical setting but not in daily life. Others have masked hypertension, where clinic values appear normal despite persistently high blood pressure outside the office. These patterns highlight why modern strategies increasingly emphasize repeated measurement, home blood pressure monitoring, and, when indicated, ambulatory blood pressure monitoring. Together, these approaches provide a more accurate picture of true blood pressure burden and improve clinical decision-making.
Home blood pressure monitoring has gained particular importance in recent years. It supports patient engagement, allows repeated assessment over time, and may help clinicians distinguish persistent hypertension from situational elevation. For patients already diagnosed with hypertension, home monitoring can improve adherence, encourage lifestyle awareness, and provide clearer data for treatment adjustment. From a public health perspective, this approach also supports decentralization of chronic disease management, especially in communities with limited access to frequent in-person care. As digital health tools continue to expand, integration of validated home devices with telemedicine and primary care follow-up may further enhance hypertension control.
Accurate technique remains a critical issue. The value of blood pressure monitoring depends not only on how often it is performed, but also on whether it is done correctly. Inaccurate cuff size, poor body positioning, inadequate rest before measurement, conversation during assessment, and use of nonvalidated devices can all produce misleading readings. For that reason, public health initiatives should not focus solely on increasing the number of measurements, but also on improving the quality of measurement practices. Training healthcare workers, educating patients, and promoting validated devices are all necessary steps in strengthening blood pressure surveillance.
The public health significance of blood pressure monitoring extends beyond diagnosis. It plays a direct role in risk stratification and long-term prevention. Persistent elevation in systolic or diastolic pressure contributes to cumulative vascular injury, endothelial dysfunction, arterial remodeling, and target organ damage. Regular monitoring allows earlier intervention through lifestyle counseling, salt reduction, weight management, physical activity, smoking cessation, and pharmacologic therapy when needed. In this way, blood pressure measurement becomes the gateway to preventing far more costly and disabling outcomes later in life.
Monitoring is also relevant at the population level because hypertension control remains uneven across regions and healthcare systems. In many low- and middle-income countries, awareness, treatment access, and continuity of care remain limited. Even in higher-resource settings, many patients diagnosed with hypertension still do not achieve recommended blood pressure targets. Public health programs that include community screening, workplace checks, pharmacy-based monitoring, and primary care follow-up can help close this gap. Such programs are especially important for high-risk groups, including older adults, individuals with diabetes, patients with obesity, and those with a family history of cardiovascular disease.
Another important dimension is the role of blood pressure monitoring in reframing prevention as an ongoing process rather than a one-time event. A single normal reading does not eliminate future risk, just as one elevated reading does not always confirm chronic hypertension. Longitudinal observation is therefore essential. This perspective is particularly relevant in public health, where continuity and repeated engagement are often more effective than isolated interventions. When monitoring is embedded into regular health behavior, it supports a culture of early detection and long-term self-management.
Scientific evidence consistently shows that improved blood pressure detection and control are associated with meaningful reductions in stroke, coronary events, heart failure, and renal disease. Yet the persistence of poorly controlled hypertension worldwide suggests that monitoring strategies are still underutilized or inconsistently implemented. Public messaging often emphasizes treatment, but monitoring itself deserves greater attention as the first practical step in prevention. Without reliable measurement, there can be no accurate diagnosis, no rational therapy adjustment, and no effective long-term control.
In conclusion, blood pressure monitoring remains a cornerstone of modern public health and cardiovascular prevention. Its value lies not only in identifying hypertension, but also in improving treatment precision, patient engagement, and long-term risk reduction. Expanding access to accurate and repeated blood pressure measurement in clinics, homes, and communities should be considered a strategic priority in efforts to reduce the global burden of cardiovascular and renal disease.
References
1. World Health Organization. Guideline for the pharmacological treatment of hypertension in adults. Geneva: WHO. 2021.
2. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Hypertension. 2018;71(6):e13-e115.
3. Unger T, Borghi C, Charchar F, et al. 2020 International Society of Hypertension Global Hypertension Practice Guidelines. Hypertension. 2020;75(6):1334-1357.
4. Stergiou GS, Palatini P, Parati G, et al. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. Journal of Hypertension. 2021;39(7):1293-1302.
5. Mills KT, Stefanescu A, He J. The global epidemiology of hypertension. Nature Reviews Nephrology. 2020;16(4):223-237.
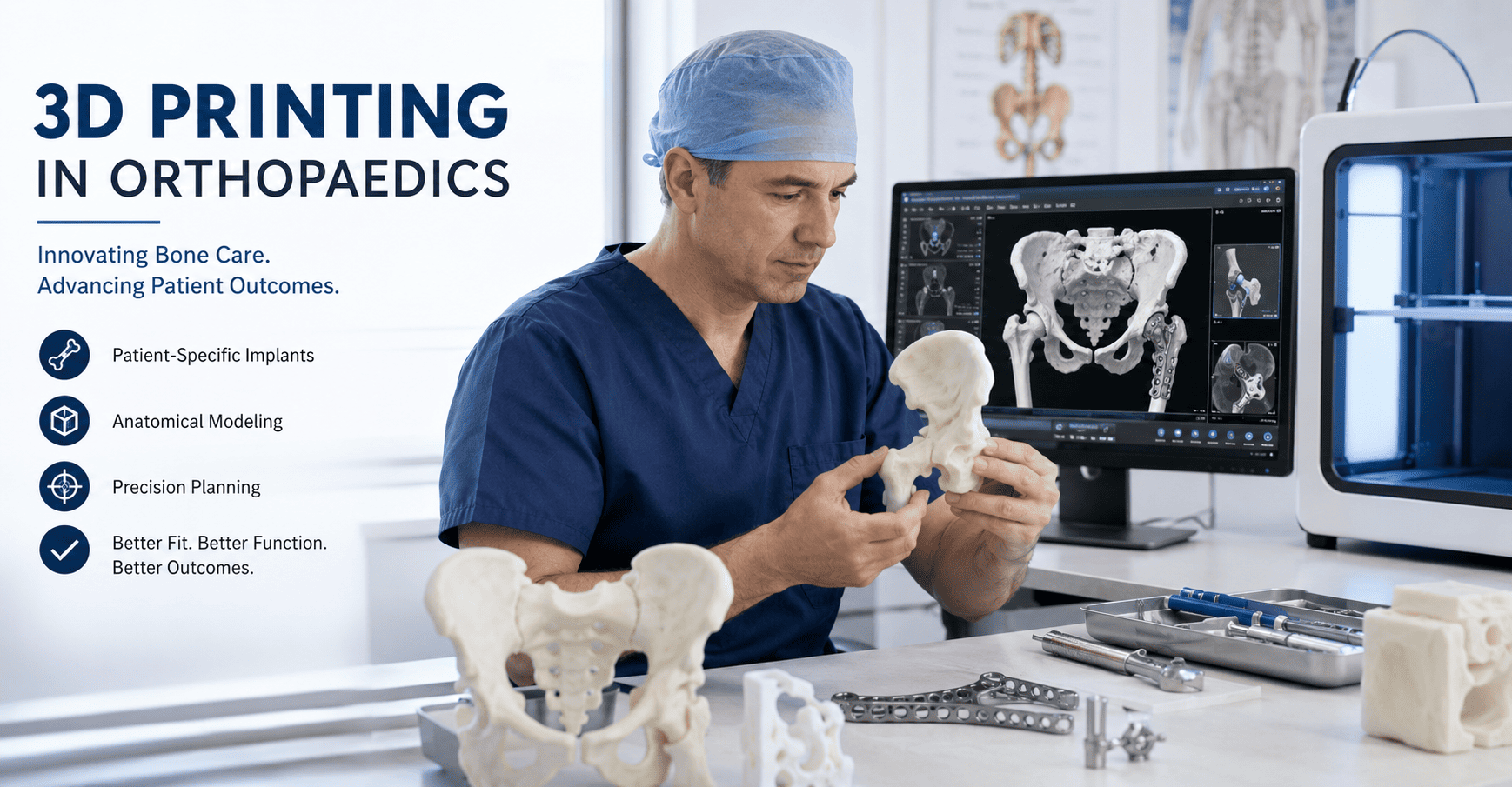
3D Printing in Orthopaedics: Expanding Precision, Personalization, and Surgical Planning in Modern Musculoskeletal Care
3D printing is increasingly reshaping orthopaedic practice by improving preoperative planning, implant customization, anatomical modeling, and educational simulation. Although challenges remain in cost, regulation, and standardization, the technology is becoming an important tool in precision musculoskeletal care.
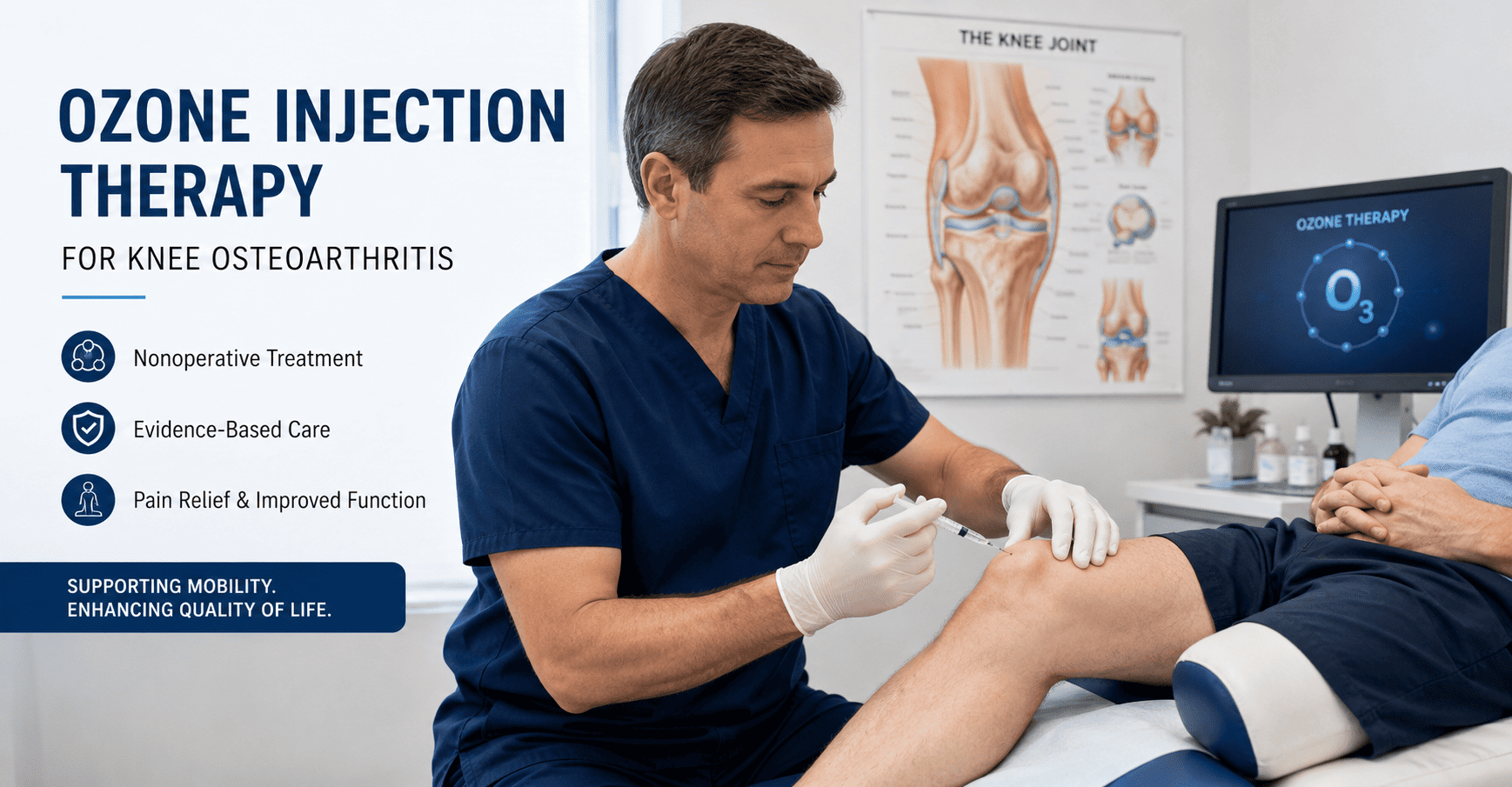
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps
Ozone injection therapy has gained attention as a nonoperative treatment option for knee osteoarthritis, particularly for short-term pain reduction and functional improvement. While early clinical findings are encouraging in selected patients, the therapy remains controversial because of inconsistent evidence quality, limited long-term data, and ongoing questions regarding standardization and comparative effectiveness.
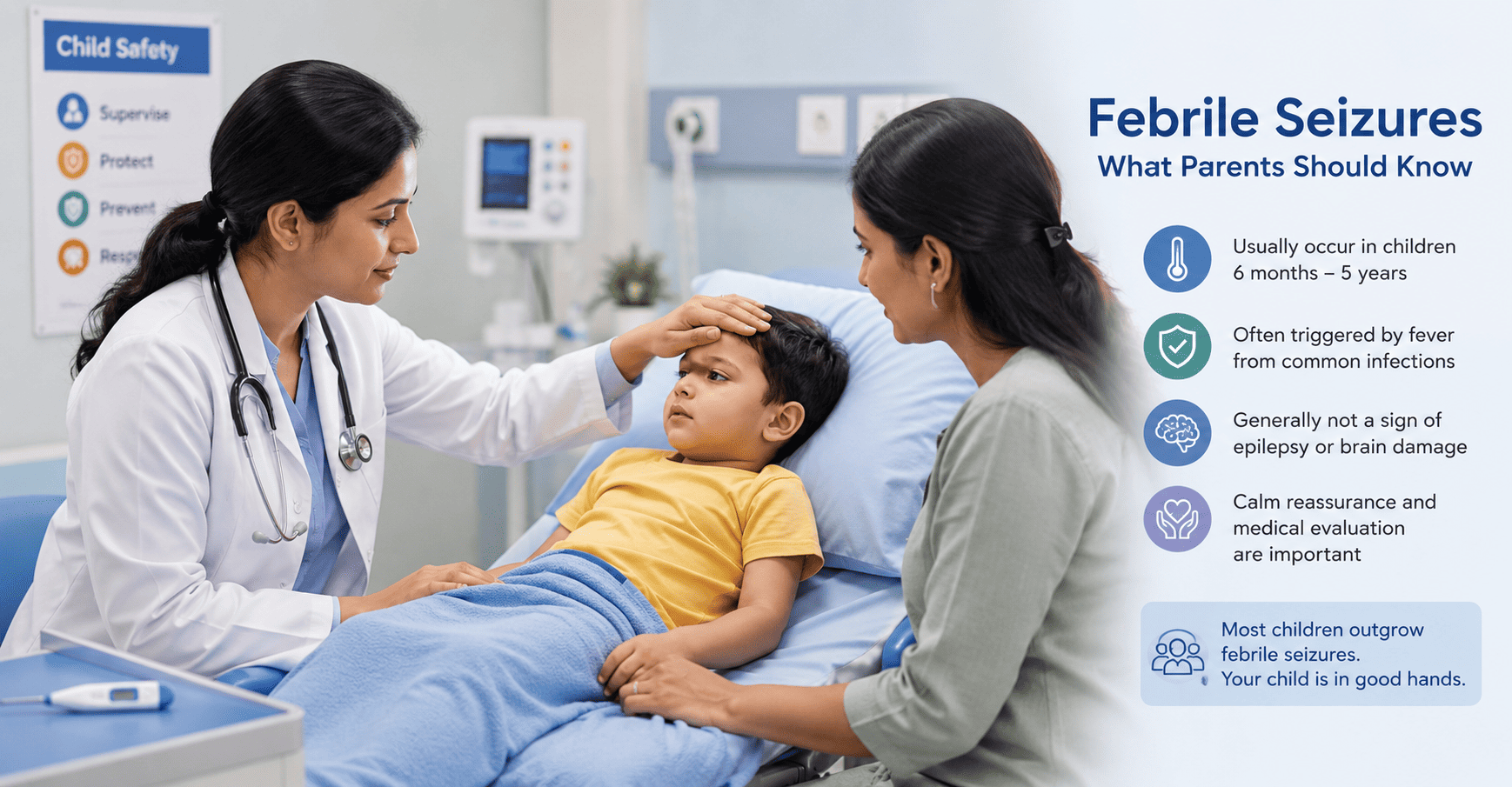
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
Febrile seizures are among the most common neurological events in early childhood and are generally associated with a favorable prognosis. Although most cases are simple and self-limited, careful clinical evaluation remains important to distinguish benign febrile seizures from central nervous system infection, epilepsy, or other serious underlying conditions.
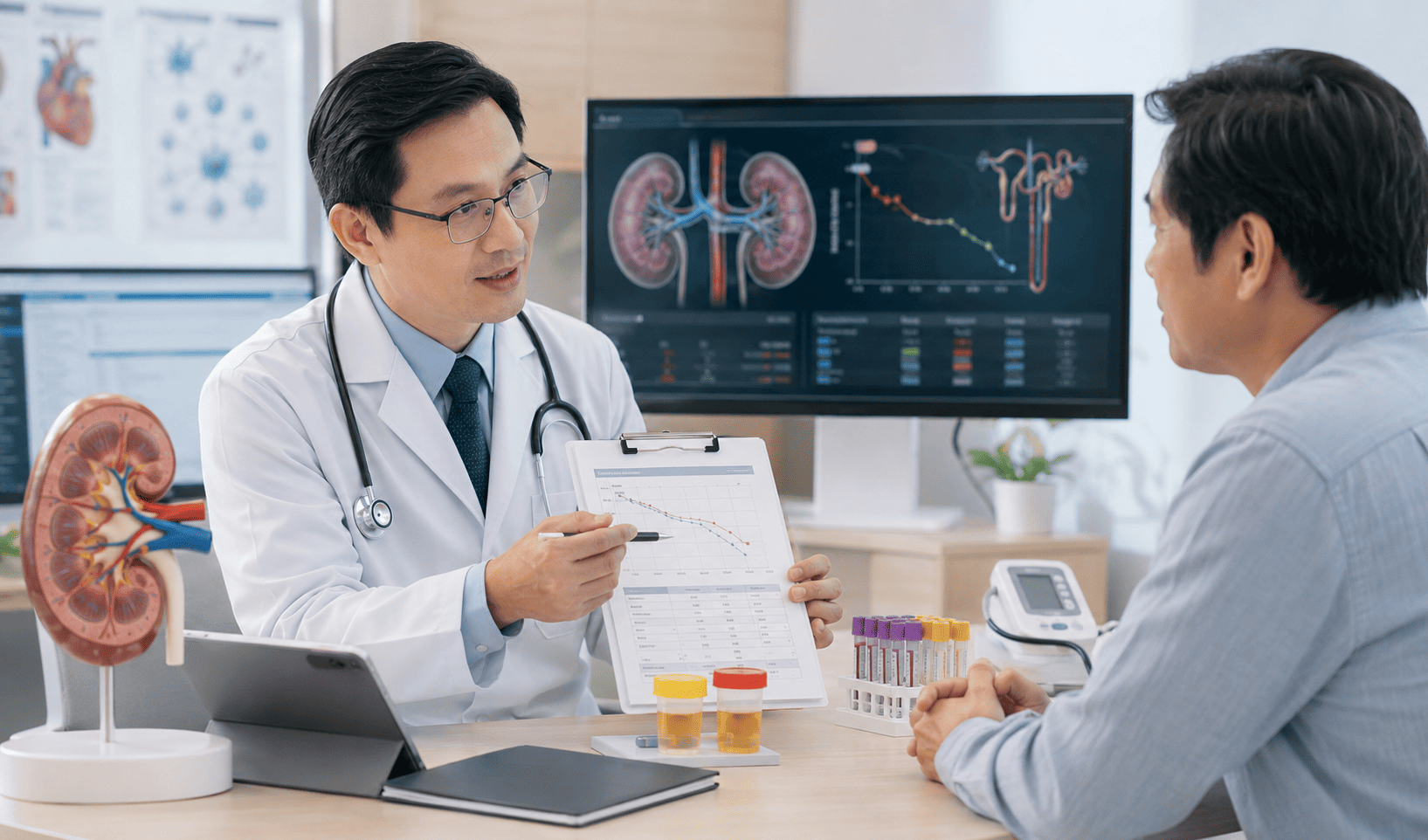
Chronic Kidney Disease: Early Detection and Risk Control Remain Central to Better Outcomes
Chronic kidney disease (CKD) continues to pose a major global health challenge due to its high prevalence, silent progression, and close association with cardiovascular complications. Early screening, timely diagnosis, and better control of diabetes and hypertension remain essential to slow disease progression and reduce kidney failure and mortality.