-
-
-
Jakarta, Indonesia
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
3D Printing in Orthopaedics: Expanding Precision, Personalization, and Surgical Planning in Modern Musculoskeletal Care
Three-dimensional printing, also known as additive manufacturing, has emerged as one of the most influential technological developments in contemporary orthopaedics. By transforming digital imaging data into physical three-dimensional models, guides, and implants, 3D printing offers new possibilities for improving surgical precision and tailoring treatment to individual anatomy. In a field where bone geometry, deformity complexity, and implant fit are central to outcomes, this technology has attracted growing attention from surgeons, engineers, and healthcare institutions worldwide.
The orthopaedic relevance of 3D printing begins with imaging integration. Computed tomography and magnetic resonance imaging data can be converted into digital models that accurately represent a patient’s skeletal structure. These reconstructions allow surgeons to inspect fracture patterns, deformities, bone loss, or tumor-related defects in far greater spatial detail than conventional two-dimensional imaging alone. When these digital reconstructions are printed into tangible anatomical models, they can improve understanding of complex cases and support more confident surgical planning.
One of the most widely recognized applications of 3D printing in orthopaedics is preoperative planning. In complex trauma, pelvic fractures, spinal deformity, limb malalignment, and revision arthroplasty, physical models can help surgeons visualize anatomy before entering the operating room. This may facilitate decisions regarding surgical approach, implant placement, osteotomy angles, and fixation strategy. In selected cases, improved planning may reduce operative time, decrease intraoperative uncertainty, and potentially minimize blood loss or fluoroscopy exposure. These practical advantages explain why 3D printing is often seen not merely as a novelty, but as an operational tool in difficult orthopaedic surgery.
Another important use is the production of patient-specific surgical guides. These guides are designed from preoperative imaging and manufactured to fit a patient’s anatomy precisely, helping direct drilling, cutting, or implant positioning. In corrective osteotomy and tumor reconstruction, this can improve technical accuracy and reproducibility. Patient-specific instrumentation has particular appeal in procedures where small alignment errors may significantly affect biomechanics or implant longevity. While such approaches require careful design validation and workflow coordination, they represent a meaningful step toward individualized orthopaedic intervention.
Beyond planning and guides, 3D printing has also expanded interest in patient-specific implants. Traditional orthopaedic implants are manufactured in standard sizes and shapes, which are effective in most routine procedures but may be less ideal in cases involving major bone defects, unusual anatomy, or revision settings. Additive manufacturing enables the design of customized implants that better match structural needs and anatomical contours. In oncology, revision arthroplasty, and major reconstructive surgery, this can be particularly valuable. Furthermore, some 3D-printed implants can be engineered with porous architectures intended to support osseointegration, which adds another layer of potential biological advantage.
The educational value of 3D printing is also significant. Anatomical models can be used to train residents, simulate rare or complex procedures, and improve communication within multidisciplinary teams. They may also help explain surgical conditions and planned interventions to patients and families in a clearer and more intuitive way. In orthopaedics, where visual-spatial understanding is essential, this educational function should not be underestimated. Better communication can improve informed consent quality and strengthen patient confidence in technically demanding care plans.
Despite these advantages, 3D printing in orthopaedics is not without limitations. Cost remains a concern, especially in resource-limited settings where imaging processing software, printing materials, technical expertise, and production infrastructure may not be readily available. Turnaround time can also be a practical barrier in urgent cases, particularly when rapid trauma decision-making is required. In addition, the quality and utility of printed models depend heavily on imaging accuracy, segmentation precision, and manufacturing standards. Poor technical workflow can reduce clinical value or even introduce error.
Regulatory and quality assurance issues are equally important. As 3D printing moves from anatomical modeling toward patient-specific implants and procedural tools, the need for validated design processes, material safety, sterilization standards, and oversight becomes increasingly critical. Unlike conventional implants produced through long-established industrial pathways, customized printed devices may require more individualized review and tighter coordination between clinicians, engineers, and manufacturers. This makes governance and standardization essential if the technology is to be integrated safely and consistently.
The scientific literature increasingly supports the usefulness of 3D printing in selected orthopaedic settings, particularly in complex surgical planning and personalized reconstruction. However, evidence is still evolving regarding long-term cost-effectiveness, broad outcome superiority, and routine use across all subspecialties. Not every orthopaedic case requires a printed model or custom implant, and the technology should not be applied indiscriminately. Its greatest value appears to lie in situations where complexity, anatomical variation, or reconstructive difficulty exceed what standard planning tools can efficiently address.
From a broader perspective, 3D printing reflects a shift in orthopaedics toward precision-based and problem-specific care. Rather than adapting every patient to standard tools alone, surgeons increasingly have access to technologies that adapt planning and hardware to the patient. This conceptual shift is especially relevant in complex deformity correction, oncologic reconstruction, and revision surgery, where individualized solutions may improve both technical execution and functional outcomes.
In summary, 3D printing is becoming an important enabling technology in modern orthopaedics. Its role in anatomical modeling, surgical planning, patient-specific guides, and customized implants highlights the growing convergence of imaging, engineering, and clinical decision-making. While cost, regulation, and standardization remain ongoing challenges, the technology is steadily moving from experimental innovation toward practical clinical application. In the years ahead, 3D printing is likely to become increasingly embedded in orthopaedic workflows that demand precision, personalization, and advanced reconstructive strategy.
References
1. Tack P, Victor J, Gemmel P, Annemans L. 3D-printing techniques in a medical setting: a systematic literature review. BioMedical Engineering OnLine. 2016;15:115.
2. Martelli N, Serrano C, van den Brink H, et al. Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery. 2016;159(6):1485-1500.
3. Vaishya R, Vijay V, Vaish A, Agarwal AK. Three-dimensional printing for complex orthopedic cases and trauma: A blessing. Apollo Medicine. 2018;15(2):51-54.
4. Yang L, Shang XW, Fan JN, et al. Application of 3D printing in the surgical planning of trimalleolar fracture and doctor-patient communication. BioMed Research International. 2016.
5. Wong KC. 3D-printed patient-specific applications in orthopedics. Orthopedic Research and Reviews. 2016;8:57-66.
The orthopaedic relevance of 3D printing begins with imaging integration. Computed tomography and magnetic resonance imaging data can be converted into digital models that accurately represent a patient’s skeletal structure. These reconstructions allow surgeons to inspect fracture patterns, deformities, bone loss, or tumor-related defects in far greater spatial detail than conventional two-dimensional imaging alone. When these digital reconstructions are printed into tangible anatomical models, they can improve understanding of complex cases and support more confident surgical planning.
One of the most widely recognized applications of 3D printing in orthopaedics is preoperative planning. In complex trauma, pelvic fractures, spinal deformity, limb malalignment, and revision arthroplasty, physical models can help surgeons visualize anatomy before entering the operating room. This may facilitate decisions regarding surgical approach, implant placement, osteotomy angles, and fixation strategy. In selected cases, improved planning may reduce operative time, decrease intraoperative uncertainty, and potentially minimize blood loss or fluoroscopy exposure. These practical advantages explain why 3D printing is often seen not merely as a novelty, but as an operational tool in difficult orthopaedic surgery.
Another important use is the production of patient-specific surgical guides. These guides are designed from preoperative imaging and manufactured to fit a patient’s anatomy precisely, helping direct drilling, cutting, or implant positioning. In corrective osteotomy and tumor reconstruction, this can improve technical accuracy and reproducibility. Patient-specific instrumentation has particular appeal in procedures where small alignment errors may significantly affect biomechanics or implant longevity. While such approaches require careful design validation and workflow coordination, they represent a meaningful step toward individualized orthopaedic intervention.
Beyond planning and guides, 3D printing has also expanded interest in patient-specific implants. Traditional orthopaedic implants are manufactured in standard sizes and shapes, which are effective in most routine procedures but may be less ideal in cases involving major bone defects, unusual anatomy, or revision settings. Additive manufacturing enables the design of customized implants that better match structural needs and anatomical contours. In oncology, revision arthroplasty, and major reconstructive surgery, this can be particularly valuable. Furthermore, some 3D-printed implants can be engineered with porous architectures intended to support osseointegration, which adds another layer of potential biological advantage.
The educational value of 3D printing is also significant. Anatomical models can be used to train residents, simulate rare or complex procedures, and improve communication within multidisciplinary teams. They may also help explain surgical conditions and planned interventions to patients and families in a clearer and more intuitive way. In orthopaedics, where visual-spatial understanding is essential, this educational function should not be underestimated. Better communication can improve informed consent quality and strengthen patient confidence in technically demanding care plans.
Despite these advantages, 3D printing in orthopaedics is not without limitations. Cost remains a concern, especially in resource-limited settings where imaging processing software, printing materials, technical expertise, and production infrastructure may not be readily available. Turnaround time can also be a practical barrier in urgent cases, particularly when rapid trauma decision-making is required. In addition, the quality and utility of printed models depend heavily on imaging accuracy, segmentation precision, and manufacturing standards. Poor technical workflow can reduce clinical value or even introduce error.
Regulatory and quality assurance issues are equally important. As 3D printing moves from anatomical modeling toward patient-specific implants and procedural tools, the need for validated design processes, material safety, sterilization standards, and oversight becomes increasingly critical. Unlike conventional implants produced through long-established industrial pathways, customized printed devices may require more individualized review and tighter coordination between clinicians, engineers, and manufacturers. This makes governance and standardization essential if the technology is to be integrated safely and consistently.
The scientific literature increasingly supports the usefulness of 3D printing in selected orthopaedic settings, particularly in complex surgical planning and personalized reconstruction. However, evidence is still evolving regarding long-term cost-effectiveness, broad outcome superiority, and routine use across all subspecialties. Not every orthopaedic case requires a printed model or custom implant, and the technology should not be applied indiscriminately. Its greatest value appears to lie in situations where complexity, anatomical variation, or reconstructive difficulty exceed what standard planning tools can efficiently address.
From a broader perspective, 3D printing reflects a shift in orthopaedics toward precision-based and problem-specific care. Rather than adapting every patient to standard tools alone, surgeons increasingly have access to technologies that adapt planning and hardware to the patient. This conceptual shift is especially relevant in complex deformity correction, oncologic reconstruction, and revision surgery, where individualized solutions may improve both technical execution and functional outcomes.
In summary, 3D printing is becoming an important enabling technology in modern orthopaedics. Its role in anatomical modeling, surgical planning, patient-specific guides, and customized implants highlights the growing convergence of imaging, engineering, and clinical decision-making. While cost, regulation, and standardization remain ongoing challenges, the technology is steadily moving from experimental innovation toward practical clinical application. In the years ahead, 3D printing is likely to become increasingly embedded in orthopaedic workflows that demand precision, personalization, and advanced reconstructive strategy.
References
1. Tack P, Victor J, Gemmel P, Annemans L. 3D-printing techniques in a medical setting: a systematic literature review. BioMedical Engineering OnLine. 2016;15:115.
2. Martelli N, Serrano C, van den Brink H, et al. Advantages and disadvantages of 3-dimensional printing in surgery: A systematic review. Surgery. 2016;159(6):1485-1500.
3. Vaishya R, Vijay V, Vaish A, Agarwal AK. Three-dimensional printing for complex orthopedic cases and trauma: A blessing. Apollo Medicine. 2018;15(2):51-54.
4. Yang L, Shang XW, Fan JN, et al. Application of 3D printing in the surgical planning of trimalleolar fracture and doctor-patient communication. BioMed Research International. 2016.
5. Wong KC. 3D-printed patient-specific applications in orthopedics. Orthopedic Research and Reviews. 2016;8:57-66.
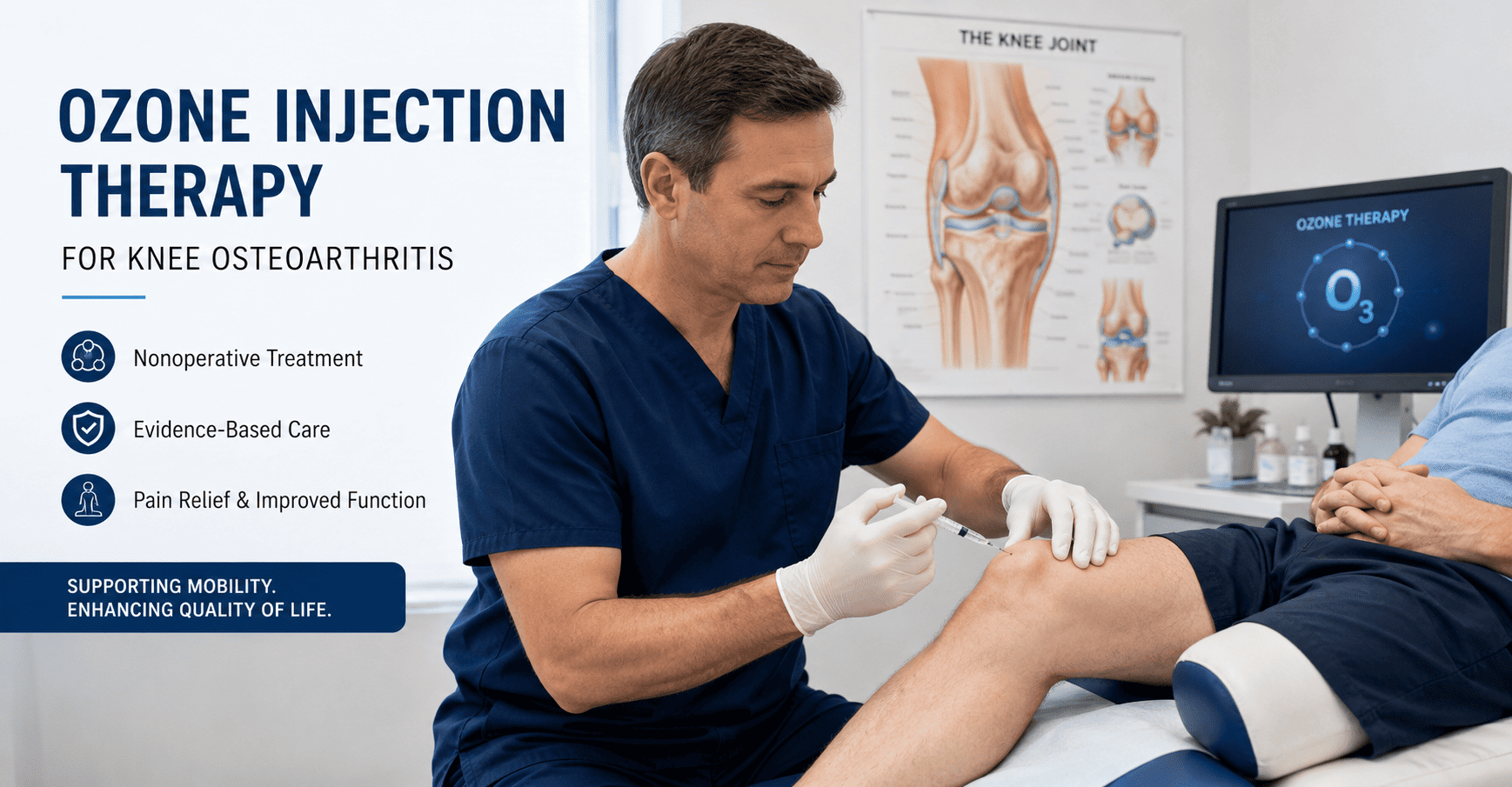
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps
Ozone injection therapy has gained attention as a nonoperative treatment option for knee osteoarthritis, particularly for short-term pain reduction and functional improvement. While early clinical findings are encouraging in selected patients, the therapy remains controversial because of inconsistent evidence quality, limited long-term data, and ongoing questions regarding standardization and comparative effectiveness.
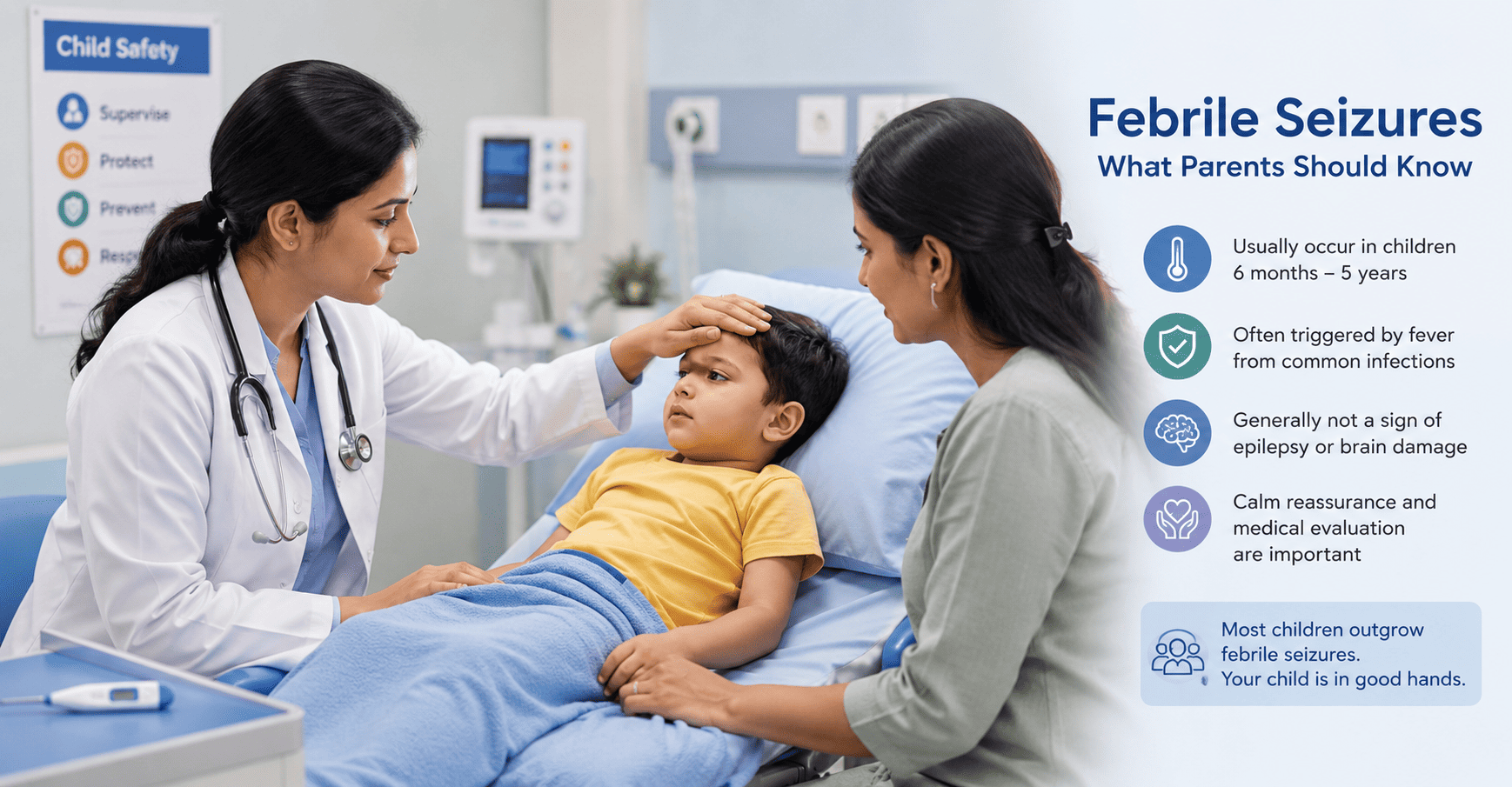
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
Febrile seizures are among the most common neurological events in early childhood and are generally associated with a favorable prognosis. Although most cases are simple and self-limited, careful clinical evaluation remains important to distinguish benign febrile seizures from central nervous system infection, epilepsy, or other serious underlying conditions.
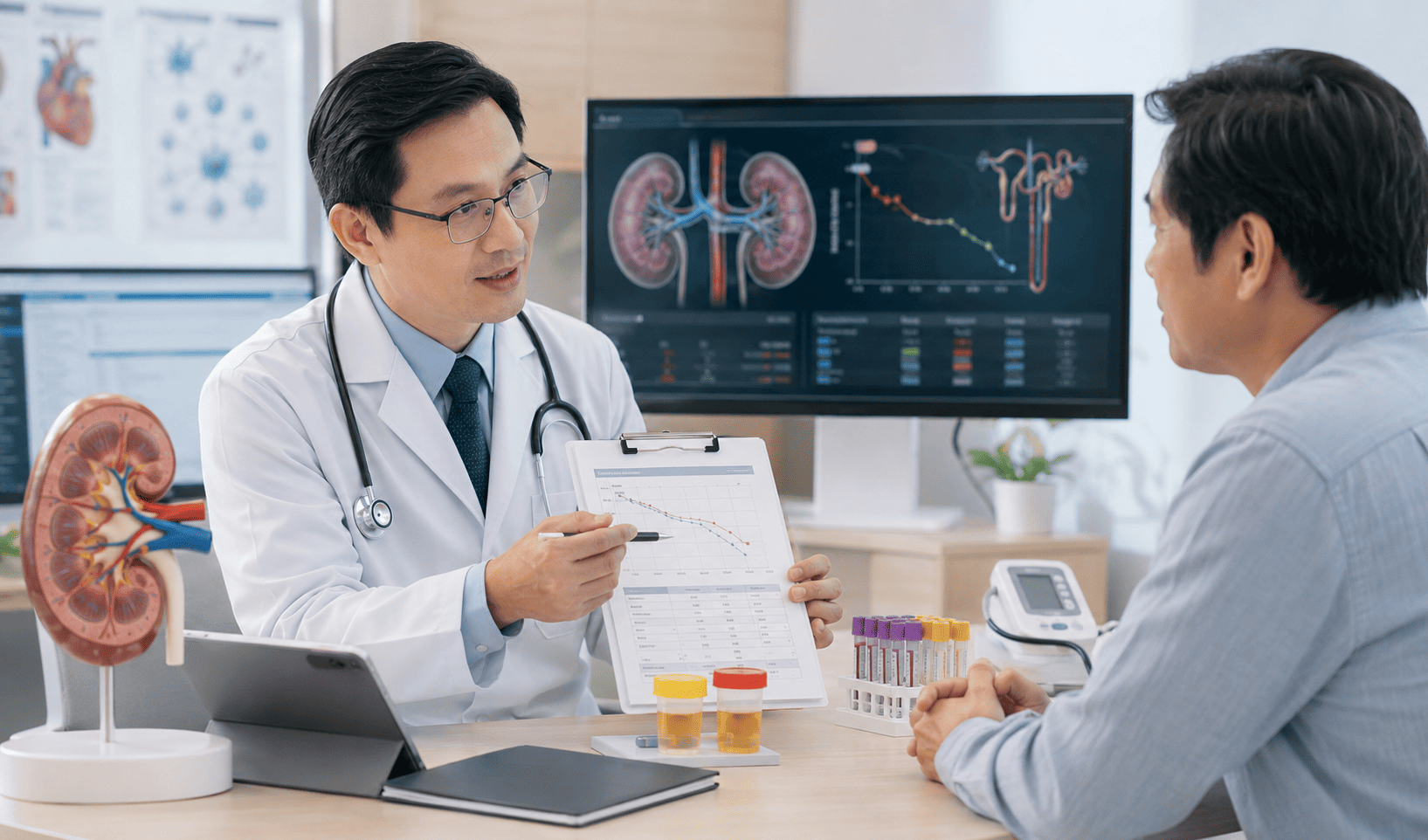
Chronic Kidney Disease: Early Detection and Risk Control Remain Central to Better Outcomes
Chronic kidney disease (CKD) continues to pose a major global health challenge due to its high prevalence, silent progression, and close association with cardiovascular complications. Early screening, timely diagnosis, and better control of diabetes and hypertension remain essential to slow disease progression and reduce kidney failure and mortality.
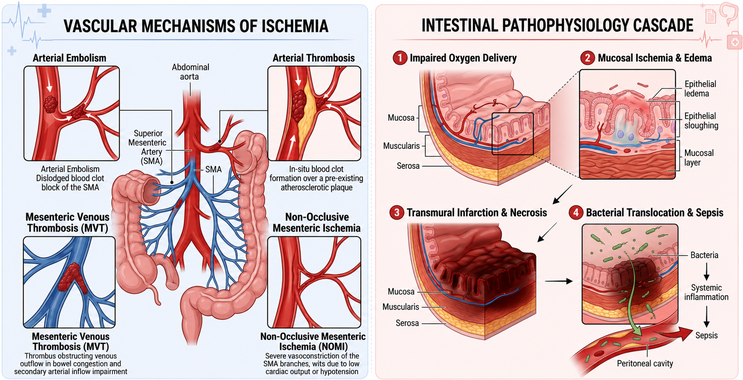
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.