-
-
-
Jakarta, Indonesia
Diabetes: A Silent Metabolic Threat That Demands Earlier Detection and Lifelong Control

Chronic Kidney Disease: Early Detection and Risk Control Remain Central to Better Outcomes
Chronic kidney disease (CKD) remains a major scientific and public health concern worldwide. It affects a large proportion of the adult population and is associated with substantial morbidity, mortality, and healthcare costs. Although CKD is widely recognized in nephrology, it is still underdiagnosed in routine care because many patients remain asymptomatic in the early stages. This delayed recognition contributes to progressive loss of kidney function, higher cardiovascular risk, and eventual kidney failure in a significant number of patients.
CKD is generally defined as an abnormality of kidney structure or function that persists for more than three months and has implications for health. In practice, the diagnosis is commonly based on decreased estimated glomerular filtration rate (eGFR), persistent albuminuria, or other evidence of kidney damage. The current international approach emphasizes both eGFR and albuminuria because these two markers are strongly associated with prognosis. Patients with reduced kidney function or elevated urinary albumin excretion face increased risks of disease progression, cardiovascular events, hospitalization, and death.
One of the major challenges in CKD is that it often develops silently. In early disease, patients may not report any obvious symptoms. Fatigue, edema, appetite loss, nausea, or changes in urination often appear only when kidney damage has become more advanced. As a result, many individuals are diagnosed late, sometimes only after complications emerge. These complications may include anemia, electrolyte imbalance, bone and mineral disorders, fluid overload, metabolic acidosis, and eventually end-stage kidney disease requiring dialysis or kidney transplantation.
The global rise of CKD is closely linked to the growing prevalence of diabetes mellitus, hypertension, obesity, and population aging. Diabetes and hypertension remain the leading causes of CKD in most regions. Chronic hyperglycemia damages the glomeruli and microvasculature, while sustained high blood pressure accelerates nephron injury and fibrosis. Older age also increases CKD risk, partly because kidney function declines gradually over time and partly because older adults frequently have multiple chronic conditions. Additional causes of CKD include glomerulonephritis, inherited kidney disorders, obstructive uropathy, recurrent acute kidney injury, and exposure to nephrotoxic medications.
CKD should not be viewed only as a kidney disorder. It is strongly associated with cardiovascular disease, and this interaction is one of the most important features of the condition. Patients with CKD have a markedly increased risk of coronary artery disease, heart failure, arrhythmia, and stroke. In fact, many individuals with CKD are more likely to die from cardiovascular causes than to reach kidney failure. This relationship means that early identification of CKD is valuable not only to preserve renal function but also to improve overall survival and reduce major cardiovascular events.
Because of its silent course, early detection is essential. Screening is particularly important in high-risk groups, including individuals with diabetes, hypertension, cardiovascular disease, obesity, family history of kidney disease, or advanced age. The most practical screening tools are serum creatinine for eGFR estimation and urine testing for albuminuria, especially the urine albumin-to-creatinine ratio. These tests are relatively accessible and provide important prognostic information. However, underuse of albuminuria testing remains a persistent problem in many healthcare settings, limiting opportunities for timely intervention.
Management of CKD focuses on slowing progression, reducing complications, and controlling associated cardiovascular risk. Blood pressure control remains a cornerstone of treatment, particularly in patients with proteinuria. Renin-angiotensin system blockade using angiotensin-converting enzyme inhibitors or angiotensin receptor blockers continues to play a central role in appropriate patients because these therapies lower intraglomerular pressure and reduce albuminuria. In patients with diabetes, glycemic control is also essential to reduce ongoing kidney injury.
Recent therapeutic advances have improved the outlook for many patients with CKD. Sodium-glucose cotransporter-2 (SGLT2) inhibitors have demonstrated significant benefits in slowing CKD progression and reducing cardiovascular outcomes in patients with and without diabetes in selected populations. These findings have reshaped the standard of care and strengthened the case for earlier diagnosis. Alongside drug therapy, nonpharmacological strategies remain important. Dietary counseling, smoking cessation, weight management, regular physical activity, and avoidance of nephrotoxic drugs are all relevant parts of comprehensive CKD care.
Despite growing scientific knowledge, substantial disparities remain in access to diagnosis and treatment. In low- and middle-income settings, laboratory limitations, low public awareness, delayed referral, and the cost of kidney replacement therapy continue to hinder effective care. Even in better-resourced systems, CKD may receive less attention than other chronic diseases despite its major long-term impact. This gap underscores the need for stronger public health strategies, including better risk-based screening, clinician education, and broader implementation of evidence-based therapies.
Overall, the scientific evidence supports a clear conclusion: CKD is common, progressive, and closely linked to premature cardiovascular and renal outcomes, yet much of its burden can be reduced through earlier detection and better risk control. Screening high-risk individuals, combining eGFR with albuminuria assessment, and initiating timely treatment are critical steps to improving outcomes. As CKD continues to expand globally, it should be treated as a primary health priority rather than a late-stage complication discovered only after irreversible damage has occurred.
References:
1. Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney International. 2024.
2. GBD Chronic Kidney Disease Collaboration. Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet. 2020;395(10225):709-733.
3. Webster AC, Nagler EV, Morton RL, Masson P. Chronic kidney disease. The Lancet. 2017;389(10075):1238-1252.
4. Heerspink HJL, Stefansson BV, Correa-Rotter R, et al. Dapagliflozin in patients with chronic kidney disease. New England Journal of Medicine. 2020;383(15):1436-1446.
5. Herrington WG, Staplin N, Wanner C, et al. Empagliflozin in patients with chronic kidney disease. New England Journal of Medicine. 2023;388:117-127.
CKD is generally defined as an abnormality of kidney structure or function that persists for more than three months and has implications for health. In practice, the diagnosis is commonly based on decreased estimated glomerular filtration rate (eGFR), persistent albuminuria, or other evidence of kidney damage. The current international approach emphasizes both eGFR and albuminuria because these two markers are strongly associated with prognosis. Patients with reduced kidney function or elevated urinary albumin excretion face increased risks of disease progression, cardiovascular events, hospitalization, and death.
One of the major challenges in CKD is that it often develops silently. In early disease, patients may not report any obvious symptoms. Fatigue, edema, appetite loss, nausea, or changes in urination often appear only when kidney damage has become more advanced. As a result, many individuals are diagnosed late, sometimes only after complications emerge. These complications may include anemia, electrolyte imbalance, bone and mineral disorders, fluid overload, metabolic acidosis, and eventually end-stage kidney disease requiring dialysis or kidney transplantation.
The global rise of CKD is closely linked to the growing prevalence of diabetes mellitus, hypertension, obesity, and population aging. Diabetes and hypertension remain the leading causes of CKD in most regions. Chronic hyperglycemia damages the glomeruli and microvasculature, while sustained high blood pressure accelerates nephron injury and fibrosis. Older age also increases CKD risk, partly because kidney function declines gradually over time and partly because older adults frequently have multiple chronic conditions. Additional causes of CKD include glomerulonephritis, inherited kidney disorders, obstructive uropathy, recurrent acute kidney injury, and exposure to nephrotoxic medications.
CKD should not be viewed only as a kidney disorder. It is strongly associated with cardiovascular disease, and this interaction is one of the most important features of the condition. Patients with CKD have a markedly increased risk of coronary artery disease, heart failure, arrhythmia, and stroke. In fact, many individuals with CKD are more likely to die from cardiovascular causes than to reach kidney failure. This relationship means that early identification of CKD is valuable not only to preserve renal function but also to improve overall survival and reduce major cardiovascular events.
Because of its silent course, early detection is essential. Screening is particularly important in high-risk groups, including individuals with diabetes, hypertension, cardiovascular disease, obesity, family history of kidney disease, or advanced age. The most practical screening tools are serum creatinine for eGFR estimation and urine testing for albuminuria, especially the urine albumin-to-creatinine ratio. These tests are relatively accessible and provide important prognostic information. However, underuse of albuminuria testing remains a persistent problem in many healthcare settings, limiting opportunities for timely intervention.
Management of CKD focuses on slowing progression, reducing complications, and controlling associated cardiovascular risk. Blood pressure control remains a cornerstone of treatment, particularly in patients with proteinuria. Renin-angiotensin system blockade using angiotensin-converting enzyme inhibitors or angiotensin receptor blockers continues to play a central role in appropriate patients because these therapies lower intraglomerular pressure and reduce albuminuria. In patients with diabetes, glycemic control is also essential to reduce ongoing kidney injury.
Recent therapeutic advances have improved the outlook for many patients with CKD. Sodium-glucose cotransporter-2 (SGLT2) inhibitors have demonstrated significant benefits in slowing CKD progression and reducing cardiovascular outcomes in patients with and without diabetes in selected populations. These findings have reshaped the standard of care and strengthened the case for earlier diagnosis. Alongside drug therapy, nonpharmacological strategies remain important. Dietary counseling, smoking cessation, weight management, regular physical activity, and avoidance of nephrotoxic drugs are all relevant parts of comprehensive CKD care.
Despite growing scientific knowledge, substantial disparities remain in access to diagnosis and treatment. In low- and middle-income settings, laboratory limitations, low public awareness, delayed referral, and the cost of kidney replacement therapy continue to hinder effective care. Even in better-resourced systems, CKD may receive less attention than other chronic diseases despite its major long-term impact. This gap underscores the need for stronger public health strategies, including better risk-based screening, clinician education, and broader implementation of evidence-based therapies.
Overall, the scientific evidence supports a clear conclusion: CKD is common, progressive, and closely linked to premature cardiovascular and renal outcomes, yet much of its burden can be reduced through earlier detection and better risk control. Screening high-risk individuals, combining eGFR with albuminuria assessment, and initiating timely treatment are critical steps to improving outcomes. As CKD continues to expand globally, it should be treated as a primary health priority rather than a late-stage complication discovered only after irreversible damage has occurred.
References:
1. Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney International. 2024.
2. GBD Chronic Kidney Disease Collaboration. Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet. 2020;395(10225):709-733.
3. Webster AC, Nagler EV, Morton RL, Masson P. Chronic kidney disease. The Lancet. 2017;389(10075):1238-1252.
4. Heerspink HJL, Stefansson BV, Correa-Rotter R, et al. Dapagliflozin in patients with chronic kidney disease. New England Journal of Medicine. 2020;383(15):1436-1446.
5. Herrington WG, Staplin N, Wanner C, et al. Empagliflozin in patients with chronic kidney disease. New England Journal of Medicine. 2023;388:117-127.
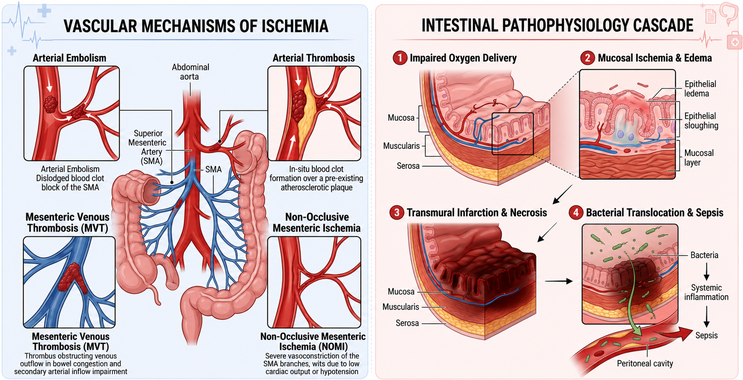
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.
Diabetes: A Silent Metabolic Threat That Demands Earlier Detection and Lifelong Control
Diabetes is no longer a disease that can be viewed only through the lens of high blood sugar. It is a chronic metabolic disorder with systemic consequences affecting the heart, kidneys, eyes, nerves, and blood vessels. Earlier detection, risk-based prevention, and sustained long-term control are essential to reducing its growing global burden.
Stroke: Why Early Recognition and Rapid Treatment Save Lives
Stroke remains one of the leading causes of death and long-term disability worldwide. Early recognition of symptoms and rapid medical treatment are essential to reduce brain injury, improve survival, and preserve quality of life.
When Is the Right Time to Get a Health Checkup?
The right time to get a health checkup is not only when symptoms appear. Evidence-based preventive screening, timed according to age, risk profile, and life stage, can help detect hypertension, colorectal cancer, breast cancer, cervical cancer, and other chronic conditions earlier—when intervention is more effective and outcomes may be better.