-
-
-
Jakarta, Indonesia
Stroke: Why Early Recognition and Rapid Treatment Save Lives
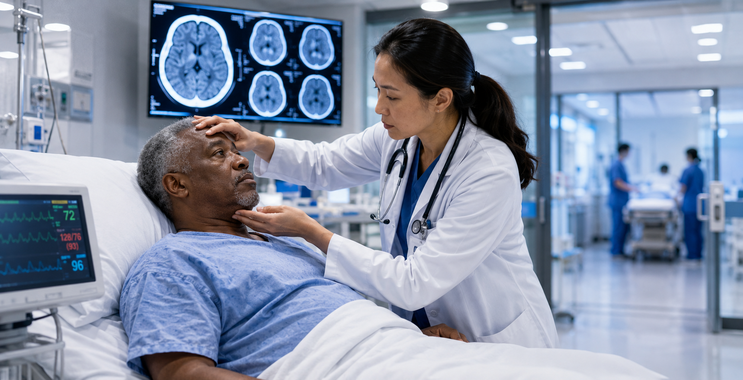
Stroke: Why Early Recognition and Rapid Treatment Save Lives
Stroke remains a major global health challenge and continues to be one of the leading causes of death and long-term disability worldwide. Despite advances in prevention, diagnosis, and treatment, many patients still arrive too late for optimal intervention. This delay is often caused by failure to recognize early warning signs, underestimation of symptom severity, or delayed transport to appropriate medical facilities. In stroke care, time is not merely important—it is decisive. The earlier a stroke is identified and treated, the greater the chance of preserving brain tissue, reducing disability, and improving survival.
A stroke occurs when blood flow to part of the brain is interrupted or when a cerebral blood vessel ruptures. The two principal forms are ischemic stroke, caused by an arterial blockage, and hemorrhagic stroke, caused by bleeding within or around the brain. Ischemic stroke accounts for the majority of cases globally. In both forms, the interruption of normal cerebral circulation deprives brain cells of oxygen and nutrients. Because neurons are highly sensitive to ischemia, irreversible injury may begin within minutes. This is the biological basis for one of the most important principles in neurology and emergency medicine: time lost is brain lost.
The clinical presentation of stroke can be sudden and dramatic, but it is not always recognized promptly by patients or families. Common warning signs include facial drooping, weakness of the arm or leg, difficulty speaking, slurred speech, confusion, visual disturbance, dizziness, imbalance, and sudden severe headache. Public education campaigns have helped promote simple recognition tools such as FAST—Face drooping, Arm weakness, Speech difficulty, Time to call emergency services. These signs are not merely educational slogans; they represent critical indicators that urgent evaluation is required. Even transient or partially improving symptoms should not be ignored, because they may represent a transient ischemic attack or an evolving stroke.
Rapid treatment has transformed the modern management of ischemic stroke. Reperfusion therapies, including intravenous thrombolysis and mechanical thrombectomy in selected patients, can significantly improve outcomes when delivered within appropriate time windows and according to established criteria. However, these therapies are highly time-dependent. Delays in symptom recognition, transport, imaging, referral, or decision-making may result in loss of eligibility for treatment. For this reason, the best stroke systems of care are those that connect public awareness, emergency response, rapid neuroimaging, and specialized clinical teams into a coordinated pathway.
Prevention remains equally important. Stroke risk is strongly associated with modifiable vascular factors such as hypertension, diabetes mellitus, dyslipidemia, smoking, obesity, atrial fibrillation, physical inactivity, and unhealthy diet. Among these, hypertension is one of the most important and consistently identified contributors to stroke risk. Effective blood pressure control, smoking cessation, appropriate diabetes management, anticoagulation when indicated for atrial fibrillation, and broader cardiovascular risk reduction all play a major role in lowering stroke incidence. In this sense, stroke prevention is inseparable from good primary care and long-term chronic disease management.
The burden of stroke extends beyond mortality alone. Many survivors experience permanent disability affecting speech, mobility, cognition, swallowing, emotional regulation, and independence in daily life. Rehabilitation therefore plays a central role after the acute phase. Multidisciplinary rehabilitation involving neurology, rehabilitation medicine, physical therapy, occupational therapy, speech therapy, nursing, and family support can substantially improve functional recovery. The degree of recovery varies widely, but earlier intervention and structured rehabilitation generally offer better results than delayed care.
From a public health perspective, stroke should be understood not only as an emergency event but also as a preventable and treatable condition that reflects broader system readiness. Communities need greater awareness, health systems need faster stroke pathways, and patients with vascular risk factors need earlier preventive intervention. The difference between full recovery and lifelong disability may depend on minutes.
In conclusion, stroke is a medical emergency that requires immediate recognition and prompt treatment. The public, clinicians, and healthcare systems all share responsibility in reducing the burden of this condition. Recognizing symptoms early, activating emergency services without delay, and addressing preventable risk factors remain the most effective strategies to save brain function, preserve independence, and save lives.
References :
1. World Health Organization. Cardiovascular diseases (CVDs). Available at: https://www.who.int
2. World Stroke Organization. Global Stroke Fact Sheet. Available at: https://www.world-stroke.org
3. Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the Early Management of Patients With Acute Ischemic Stroke. Stroke. American Heart Association.
4. Feigin VL, Brainin M, Norrving B, et al. World Stroke Organization Global Stroke Fact Sheet.
5. Centers for Disease Control and Prevention. Stroke Facts. Available at: https://www.cdc.gov
A stroke occurs when blood flow to part of the brain is interrupted or when a cerebral blood vessel ruptures. The two principal forms are ischemic stroke, caused by an arterial blockage, and hemorrhagic stroke, caused by bleeding within or around the brain. Ischemic stroke accounts for the majority of cases globally. In both forms, the interruption of normal cerebral circulation deprives brain cells of oxygen and nutrients. Because neurons are highly sensitive to ischemia, irreversible injury may begin within minutes. This is the biological basis for one of the most important principles in neurology and emergency medicine: time lost is brain lost.
The clinical presentation of stroke can be sudden and dramatic, but it is not always recognized promptly by patients or families. Common warning signs include facial drooping, weakness of the arm or leg, difficulty speaking, slurred speech, confusion, visual disturbance, dizziness, imbalance, and sudden severe headache. Public education campaigns have helped promote simple recognition tools such as FAST—Face drooping, Arm weakness, Speech difficulty, Time to call emergency services. These signs are not merely educational slogans; they represent critical indicators that urgent evaluation is required. Even transient or partially improving symptoms should not be ignored, because they may represent a transient ischemic attack or an evolving stroke.
Rapid treatment has transformed the modern management of ischemic stroke. Reperfusion therapies, including intravenous thrombolysis and mechanical thrombectomy in selected patients, can significantly improve outcomes when delivered within appropriate time windows and according to established criteria. However, these therapies are highly time-dependent. Delays in symptom recognition, transport, imaging, referral, or decision-making may result in loss of eligibility for treatment. For this reason, the best stroke systems of care are those that connect public awareness, emergency response, rapid neuroimaging, and specialized clinical teams into a coordinated pathway.
Prevention remains equally important. Stroke risk is strongly associated with modifiable vascular factors such as hypertension, diabetes mellitus, dyslipidemia, smoking, obesity, atrial fibrillation, physical inactivity, and unhealthy diet. Among these, hypertension is one of the most important and consistently identified contributors to stroke risk. Effective blood pressure control, smoking cessation, appropriate diabetes management, anticoagulation when indicated for atrial fibrillation, and broader cardiovascular risk reduction all play a major role in lowering stroke incidence. In this sense, stroke prevention is inseparable from good primary care and long-term chronic disease management.
The burden of stroke extends beyond mortality alone. Many survivors experience permanent disability affecting speech, mobility, cognition, swallowing, emotional regulation, and independence in daily life. Rehabilitation therefore plays a central role after the acute phase. Multidisciplinary rehabilitation involving neurology, rehabilitation medicine, physical therapy, occupational therapy, speech therapy, nursing, and family support can substantially improve functional recovery. The degree of recovery varies widely, but earlier intervention and structured rehabilitation generally offer better results than delayed care.
From a public health perspective, stroke should be understood not only as an emergency event but also as a preventable and treatable condition that reflects broader system readiness. Communities need greater awareness, health systems need faster stroke pathways, and patients with vascular risk factors need earlier preventive intervention. The difference between full recovery and lifelong disability may depend on minutes.
In conclusion, stroke is a medical emergency that requires immediate recognition and prompt treatment. The public, clinicians, and healthcare systems all share responsibility in reducing the burden of this condition. Recognizing symptoms early, activating emergency services without delay, and addressing preventable risk factors remain the most effective strategies to save brain function, preserve independence, and save lives.
References :
1. World Health Organization. Cardiovascular diseases (CVDs). Available at: https://www.who.int
2. World Stroke Organization. Global Stroke Fact Sheet. Available at: https://www.world-stroke.org
3. Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the Early Management of Patients With Acute Ischemic Stroke. Stroke. American Heart Association.
4. Feigin VL, Brainin M, Norrving B, et al. World Stroke Organization Global Stroke Fact Sheet.
5. Centers for Disease Control and Prevention. Stroke Facts. Available at: https://www.cdc.gov
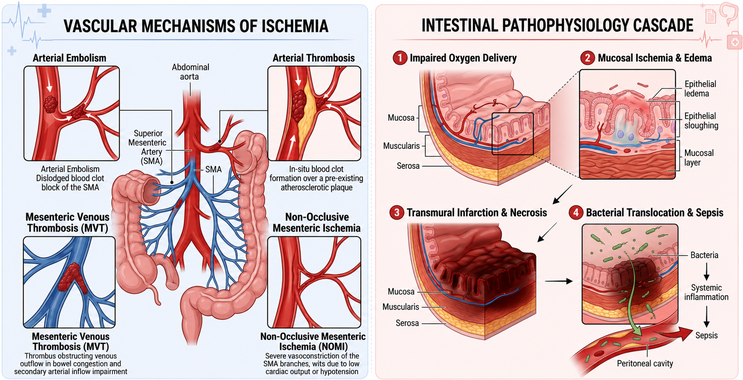
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.
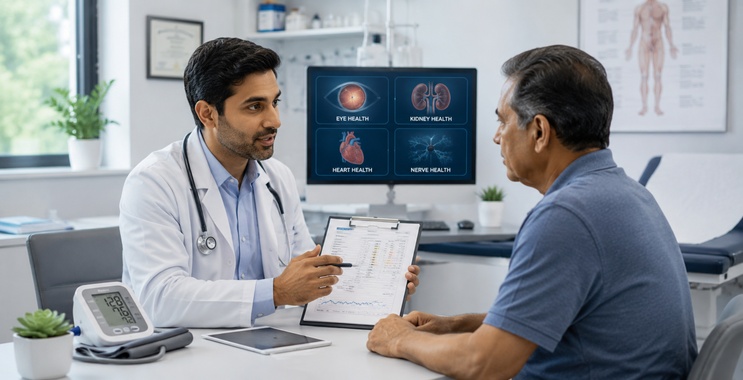
Diabetes: A Silent Metabolic Threat That Demands Earlier Detection and Lifelong Control
Diabetes is no longer a disease that can be viewed only through the lens of high blood sugar. It is a chronic metabolic disorder with systemic consequences affecting the heart, kidneys, eyes, nerves, and blood vessels. Earlier detection, risk-based prevention, and sustained long-term control are essential to reducing its growing global burden.
When Is the Right Time to Get a Health Checkup?
The right time to get a health checkup is not only when symptoms appear. Evidence-based preventive screening, timed according to age, risk profile, and life stage, can help detect hypertension, colorectal cancer, breast cancer, cervical cancer, and other chronic conditions earlier—when intervention is more effective and outcomes may be better.