-
-
-
Jakarta, Indonesia
Stroke: Why Early Recognition and Rapid Treatment Save Lives
Diabetes: A Silent Metabolic Threat That Demands Earlier Detection and Lifelong Control
Diabetes has become one of the defining chronic diseases of modern medicine, not only because of its rising prevalence, but also because of the breadth of organ damage it can produce over time. For many people, diabetes begins quietly. Symptoms may be absent, vague, or ignored for years, especially in type 2 diabetes. Yet beneath this seemingly silent phase, chronic hyperglycemia may already be affecting blood vessels, nerves, kidneys, the retina, and the cardiovascular system. This is precisely why diabetes deserves to be discussed not merely as a disease of “sugar,” but as a systemic metabolic disorder that requires earlier recognition and more sustained long-term control.
The global burden is substantial and still increasing. According to the World Health Organization, the number of people living with diabetes rose from 200 million in 1990 to 830 million in 2022, with prevalence increasing more rapidly in low- and middle-income countries than in high-income settings. WHO also reports that diabetes contributes directly to mortality and indirectly to cardiovascular and kidney-related deaths, while long-term complications include blindness, kidney failure, stroke, myocardial infarction, and lower-limb amputation. These figures make clear that diabetes is not simply common; it is a major driver of premature disability and health-system strain.
Clinically, diabetes is heterogeneous. Type 1 diabetes results from severe insulin deficiency, usually due to autoimmune destruction of pancreatic beta cells, and requires insulin for survival. Type 2 diabetes, which accounts for the great majority of adult cases worldwide, develops through a complex interaction of insulin resistance, progressive beta-cell dysfunction, excess adiposity, genetic susceptibility, and environmental exposures. Gestational diabetes adds another important dimension because it affects both maternal and fetal outcomes and increases future metabolic risk for mother and child. Modern classification systems emphasize that diabetes is not a single uniform disease, and this distinction matters because diagnosis, treatment intensity, and long-term risk differ across subtypes.
One of the most important public health challenges is that type 2 diabetes may remain undiagnosed for years. During that interval, many patients already pass through a stage of prediabetes or early dysglycemia, when prevention or delay may still be possible. The American Diabetes Association Standards of Care continue to emphasize structured diagnosis and classification, because accurate identification is the foundation of appropriate treatment. This is particularly relevant in adults whose phenotype does not fit neatly into traditional assumptions. Age alone, body habitus alone, or symptom severity alone should not be used as simplistic diagnostic shortcuts.
For the general public, the critical message is that diabetes often does not announce itself dramatically. Although classic symptoms such as polydipsia, polyuria, fatigue, blurred vision, and unintentional weight loss are well recognized, many patients with type 2 diabetes experience only mild or nonspecific complaints. Some are first diagnosed only after complications emerge, such as neuropathic symptoms, recurrent infections, renal impairment, or a cardiovascular event. This delayed recognition is dangerous because earlier diagnosis is associated with earlier intervention, and earlier intervention creates a wider opportunity to reduce cumulative vascular injury.
The reason diabetes is so clinically important lies in its complications. Chronic hyperglycemia promotes both microvascular and macrovascular disease. At the microvascular level, diabetes is strongly linked to retinopathy, nephropathy, and neuropathy. At the macrovascular level, it substantially increases the risk of myocardial infarction, stroke, peripheral arterial disease, heart failure, and premature death. In practical terms, this means that diabetes management cannot be reduced to a single glucose number. Good care must include glycemic control, blood pressure management, lipid control, kidney risk surveillance, retinal assessment, foot care, and cardiovascular risk reduction. Contemporary diabetes care is therefore multidisciplinary by nature.
This broader view of diabetes is strongly reflected in current evidence-based guidance. The American Diabetes Association’s 2024 Standards of Care devote separate sections to diagnosis and classification, cardiovascular disease and risk management, chronic kidney disease and risk management, and retinopathy, neuropathy, and foot care. That structure itself is revealing: diabetes is no longer managed adequately by focusing on hyperglycemia alone. Instead, modern care addresses the full spectrum of metabolic and vascular risk. This shift is one of the most important developments in contemporary endocrinology.
Another major development is the recognition that treatment decisions should be guided not only by glycemic targets, but also by comorbid cardiovascular and renal risk. Large cardiovascular outcome trials and subsequent meta-analyses have shown that some glucose-lowering therapies, particularly GLP-1 receptor agonists and SGLT2 inhibitors, offer benefits that extend beyond glucose reduction alone. For patients with type 2 diabetes and high cardiovascular or kidney risk, this has changed the therapeutic conversation. In other words, choosing diabetes therapy is no longer simply a matter of lowering blood sugar as much as possible; it is also about selecting agents that improve long-term outcomes in organs most threatened by the disease.
At the population level, prevention remains indispensable. A large proportion of type 2 diabetes is linked to modifiable risk factors such as obesity, physical inactivity, poor dietary pattern, and metabolic syndrome. Weight reduction, especially when clinically meaningful and sustained, can reduce diabetes risk and improve glycemic control, and in selected patients may even contribute to remission. This has led to increased interest in intensive lifestyle intervention, obesity treatment, and the interface between endocrinology and cardiovascular prevention. For the public, this is an encouraging point: diabetes is serious, but part of its trajectory is modifiable, especially when intervention begins early.
Still, the message should not be oversimplified into lifestyle advice alone. Diabetes is not merely a consequence of “eating too much sugar,” nor should it be framed as a moral failure of self-control. Such reductionism is both scientifically incomplete and socially harmful. Diabetes arises from a complex interaction of biology, behavior, family history, adiposity, socioeconomic context, and health-system access. Effective prevention and treatment therefore require both personal engagement and structural support, including access to screening, medication, counseling, and long-term follow-up.
Screening also deserves emphasis. Many adults at elevated risk remain untested until disease is established. This is especially concerning because prediabetes and type 2 diabetes frequently coexist with hypertension, dyslipidemia, and obesity, multiplying cardiovascular risk. For that reason, risk-based screening and regular medical follow-up are essential, particularly in adults with excess weight, sedentary lifestyles, prior gestational diabetes, family history, or other metabolic risk factors. The principle is straightforward: if diabetes is often silent early in its course, then waiting for obvious symptoms is a clinically poor strategy.
For people already diagnosed, the long-term goal is not merely survival, but preservation of function and quality of life. Preventing vision loss, dialysis, foot ulceration, amputation, disabling neuropathy, stroke, and heart failure is just as important as lowering glycated hemoglobin. This is why regular retinal evaluation, kidney assessment, foot examination, and cardiovascular risk management are central to comprehensive care. Diabetes is a disease that rewards consistency: consistent monitoring, consistent treatment, and consistent engagement between patient and clinician.
In conclusion, diabetes should be understood as a chronic systemic disorder with far-reaching consequences rather than a narrowly defined disturbance of blood glucose. It often progresses silently, it damages multiple organ systems, and it imposes a major burden on individuals and societies alike. Yet it is also a disease in which earlier diagnosis, evidence-based treatment, risk-factor modification, and structured follow-up can meaningfully change outcomes. For the public, the most important message is simple but powerful: diabetes is common, serious, and often quiet—but it is not beyond control when detected early and managed well.
References :
1. World Health Organization. Diabetes fact sheet. Available at: https://www.who.int/news-room/fact-sheets/detail/diabetes
2. Centers for Disease Control and Prevention. Diabetes Basics. Available at: https://www.cdc.gov/diabetes/about/index.html
3. American Diabetes Association Professional Practice Committee. 2. Diagnosis and Classification of Diabetes: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1). PMID: 38078589.
4. American Diabetes Association Professional Practice Committee. 10. Cardiovascular Disease and Risk Management: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S179-S218. doi:10.2337/dc24-S010. PMID: 38078592.
5. American Diabetes Association Professional Practice Committee. 11. Chronic Kidney Disease and Risk Management: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S219-S230. doi:10.2337/dc24-S011. PMID: 38078574.
6. American Diabetes Association Professional Practice Committee. 12. Retinopathy, Neuropathy, and Foot Care: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S231-S243. doi:10.2337/dc24-S012. PMID: 38078577.
7. Sattar N, Lee MMY, Kristensen SL, et al. Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of randomised trials. Lancet Diabetes Endocrinol. 2021;9(10):653-662. doi:10.1016/S2213-8587(21)00203-5. PMID: 34425083.
8. Sweeting A, Hannah W, Backman H, et al. Epidemiology and management of gestational diabetes. Lancet. 2024;404(10448):175-192. doi:10.1016/S0140-6736(24)00825-0. PMID: 38909620.
9. Perdomo CM, Cohen RV, Sumithran P, Clément K, Frühbeck G. Contemporary medical, device, and surgical therapies for obesity in adults. Lancet. 2023;401(10382):1116-1130. doi:10.1016/S0140-6736(22)02403-5. PMID: 36774932.
10. Tonga E, Worboys H, Evans RA, et al. Physical activity guidelines for adults with type 2 diabetes: Systematic review. Diabetes Res Clin Pract. 2025;220:111982. doi:10.1016/j.diabres.2024.111982. PMID: 39746550.
11. Kanbour S, Ageeb RA, Malik RA, Abu-Raddad LJ. Impact of bodyweight loss on type 2 diabetes remission: a systematic review and meta-regression analysis of randomised controlled trials. Lancet Diabetes Endocrinol. 2025;13(4):294-306. doi:10.1016/S2213-8587(24)00346-2.
12. Holt RIG, DeVries JH, Hess-Fischl A, et al. The management of type 1 diabetes in adults. Nat Rev Dis Primers. 2021;7:69. doi:10.1038/s41572-021-00284-2.
The global burden is substantial and still increasing. According to the World Health Organization, the number of people living with diabetes rose from 200 million in 1990 to 830 million in 2022, with prevalence increasing more rapidly in low- and middle-income countries than in high-income settings. WHO also reports that diabetes contributes directly to mortality and indirectly to cardiovascular and kidney-related deaths, while long-term complications include blindness, kidney failure, stroke, myocardial infarction, and lower-limb amputation. These figures make clear that diabetes is not simply common; it is a major driver of premature disability and health-system strain.
Clinically, diabetes is heterogeneous. Type 1 diabetes results from severe insulin deficiency, usually due to autoimmune destruction of pancreatic beta cells, and requires insulin for survival. Type 2 diabetes, which accounts for the great majority of adult cases worldwide, develops through a complex interaction of insulin resistance, progressive beta-cell dysfunction, excess adiposity, genetic susceptibility, and environmental exposures. Gestational diabetes adds another important dimension because it affects both maternal and fetal outcomes and increases future metabolic risk for mother and child. Modern classification systems emphasize that diabetes is not a single uniform disease, and this distinction matters because diagnosis, treatment intensity, and long-term risk differ across subtypes.
One of the most important public health challenges is that type 2 diabetes may remain undiagnosed for years. During that interval, many patients already pass through a stage of prediabetes or early dysglycemia, when prevention or delay may still be possible. The American Diabetes Association Standards of Care continue to emphasize structured diagnosis and classification, because accurate identification is the foundation of appropriate treatment. This is particularly relevant in adults whose phenotype does not fit neatly into traditional assumptions. Age alone, body habitus alone, or symptom severity alone should not be used as simplistic diagnostic shortcuts.
For the general public, the critical message is that diabetes often does not announce itself dramatically. Although classic symptoms such as polydipsia, polyuria, fatigue, blurred vision, and unintentional weight loss are well recognized, many patients with type 2 diabetes experience only mild or nonspecific complaints. Some are first diagnosed only after complications emerge, such as neuropathic symptoms, recurrent infections, renal impairment, or a cardiovascular event. This delayed recognition is dangerous because earlier diagnosis is associated with earlier intervention, and earlier intervention creates a wider opportunity to reduce cumulative vascular injury.
The reason diabetes is so clinically important lies in its complications. Chronic hyperglycemia promotes both microvascular and macrovascular disease. At the microvascular level, diabetes is strongly linked to retinopathy, nephropathy, and neuropathy. At the macrovascular level, it substantially increases the risk of myocardial infarction, stroke, peripheral arterial disease, heart failure, and premature death. In practical terms, this means that diabetes management cannot be reduced to a single glucose number. Good care must include glycemic control, blood pressure management, lipid control, kidney risk surveillance, retinal assessment, foot care, and cardiovascular risk reduction. Contemporary diabetes care is therefore multidisciplinary by nature.
This broader view of diabetes is strongly reflected in current evidence-based guidance. The American Diabetes Association’s 2024 Standards of Care devote separate sections to diagnosis and classification, cardiovascular disease and risk management, chronic kidney disease and risk management, and retinopathy, neuropathy, and foot care. That structure itself is revealing: diabetes is no longer managed adequately by focusing on hyperglycemia alone. Instead, modern care addresses the full spectrum of metabolic and vascular risk. This shift is one of the most important developments in contemporary endocrinology.
Another major development is the recognition that treatment decisions should be guided not only by glycemic targets, but also by comorbid cardiovascular and renal risk. Large cardiovascular outcome trials and subsequent meta-analyses have shown that some glucose-lowering therapies, particularly GLP-1 receptor agonists and SGLT2 inhibitors, offer benefits that extend beyond glucose reduction alone. For patients with type 2 diabetes and high cardiovascular or kidney risk, this has changed the therapeutic conversation. In other words, choosing diabetes therapy is no longer simply a matter of lowering blood sugar as much as possible; it is also about selecting agents that improve long-term outcomes in organs most threatened by the disease.
At the population level, prevention remains indispensable. A large proportion of type 2 diabetes is linked to modifiable risk factors such as obesity, physical inactivity, poor dietary pattern, and metabolic syndrome. Weight reduction, especially when clinically meaningful and sustained, can reduce diabetes risk and improve glycemic control, and in selected patients may even contribute to remission. This has led to increased interest in intensive lifestyle intervention, obesity treatment, and the interface between endocrinology and cardiovascular prevention. For the public, this is an encouraging point: diabetes is serious, but part of its trajectory is modifiable, especially when intervention begins early.
Still, the message should not be oversimplified into lifestyle advice alone. Diabetes is not merely a consequence of “eating too much sugar,” nor should it be framed as a moral failure of self-control. Such reductionism is both scientifically incomplete and socially harmful. Diabetes arises from a complex interaction of biology, behavior, family history, adiposity, socioeconomic context, and health-system access. Effective prevention and treatment therefore require both personal engagement and structural support, including access to screening, medication, counseling, and long-term follow-up.
Screening also deserves emphasis. Many adults at elevated risk remain untested until disease is established. This is especially concerning because prediabetes and type 2 diabetes frequently coexist with hypertension, dyslipidemia, and obesity, multiplying cardiovascular risk. For that reason, risk-based screening and regular medical follow-up are essential, particularly in adults with excess weight, sedentary lifestyles, prior gestational diabetes, family history, or other metabolic risk factors. The principle is straightforward: if diabetes is often silent early in its course, then waiting for obvious symptoms is a clinically poor strategy.
For people already diagnosed, the long-term goal is not merely survival, but preservation of function and quality of life. Preventing vision loss, dialysis, foot ulceration, amputation, disabling neuropathy, stroke, and heart failure is just as important as lowering glycated hemoglobin. This is why regular retinal evaluation, kidney assessment, foot examination, and cardiovascular risk management are central to comprehensive care. Diabetes is a disease that rewards consistency: consistent monitoring, consistent treatment, and consistent engagement between patient and clinician.
In conclusion, diabetes should be understood as a chronic systemic disorder with far-reaching consequences rather than a narrowly defined disturbance of blood glucose. It often progresses silently, it damages multiple organ systems, and it imposes a major burden on individuals and societies alike. Yet it is also a disease in which earlier diagnosis, evidence-based treatment, risk-factor modification, and structured follow-up can meaningfully change outcomes. For the public, the most important message is simple but powerful: diabetes is common, serious, and often quiet—but it is not beyond control when detected early and managed well.
References :
1. World Health Organization. Diabetes fact sheet. Available at: https://www.who.int/news-room/fact-sheets/detail/diabetes
2. Centers for Disease Control and Prevention. Diabetes Basics. Available at: https://www.cdc.gov/diabetes/about/index.html
3. American Diabetes Association Professional Practice Committee. 2. Diagnosis and Classification of Diabetes: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1). PMID: 38078589.
4. American Diabetes Association Professional Practice Committee. 10. Cardiovascular Disease and Risk Management: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S179-S218. doi:10.2337/dc24-S010. PMID: 38078592.
5. American Diabetes Association Professional Practice Committee. 11. Chronic Kidney Disease and Risk Management: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S219-S230. doi:10.2337/dc24-S011. PMID: 38078574.
6. American Diabetes Association Professional Practice Committee. 12. Retinopathy, Neuropathy, and Foot Care: Standards of Care in Diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S231-S243. doi:10.2337/dc24-S012. PMID: 38078577.
7. Sattar N, Lee MMY, Kristensen SL, et al. Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of randomised trials. Lancet Diabetes Endocrinol. 2021;9(10):653-662. doi:10.1016/S2213-8587(21)00203-5. PMID: 34425083.
8. Sweeting A, Hannah W, Backman H, et al. Epidemiology and management of gestational diabetes. Lancet. 2024;404(10448):175-192. doi:10.1016/S0140-6736(24)00825-0. PMID: 38909620.
9. Perdomo CM, Cohen RV, Sumithran P, Clément K, Frühbeck G. Contemporary medical, device, and surgical therapies for obesity in adults. Lancet. 2023;401(10382):1116-1130. doi:10.1016/S0140-6736(22)02403-5. PMID: 36774932.
10. Tonga E, Worboys H, Evans RA, et al. Physical activity guidelines for adults with type 2 diabetes: Systematic review. Diabetes Res Clin Pract. 2025;220:111982. doi:10.1016/j.diabres.2024.111982. PMID: 39746550.
11. Kanbour S, Ageeb RA, Malik RA, Abu-Raddad LJ. Impact of bodyweight loss on type 2 diabetes remission: a systematic review and meta-regression analysis of randomised controlled trials. Lancet Diabetes Endocrinol. 2025;13(4):294-306. doi:10.1016/S2213-8587(24)00346-2.
12. Holt RIG, DeVries JH, Hess-Fischl A, et al. The management of type 1 diabetes in adults. Nat Rev Dis Primers. 2021;7:69. doi:10.1038/s41572-021-00284-2.
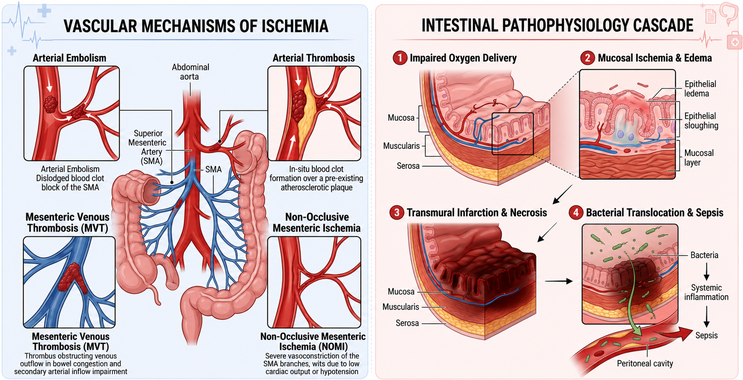
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.
Stroke: Why Early Recognition and Rapid Treatment Save Lives
Stroke remains one of the leading causes of death and long-term disability worldwide. Early recognition of symptoms and rapid medical treatment are essential to reduce brain injury, improve survival, and preserve quality of life.
When Is the Right Time to Get a Health Checkup?
The right time to get a health checkup is not only when symptoms appear. Evidence-based preventive screening, timed according to age, risk profile, and life stage, can help detect hypertension, colorectal cancer, breast cancer, cervical cancer, and other chronic conditions earlier—when intervention is more effective and outcomes may be better.