-
-
-
Jakarta, Indonesia
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
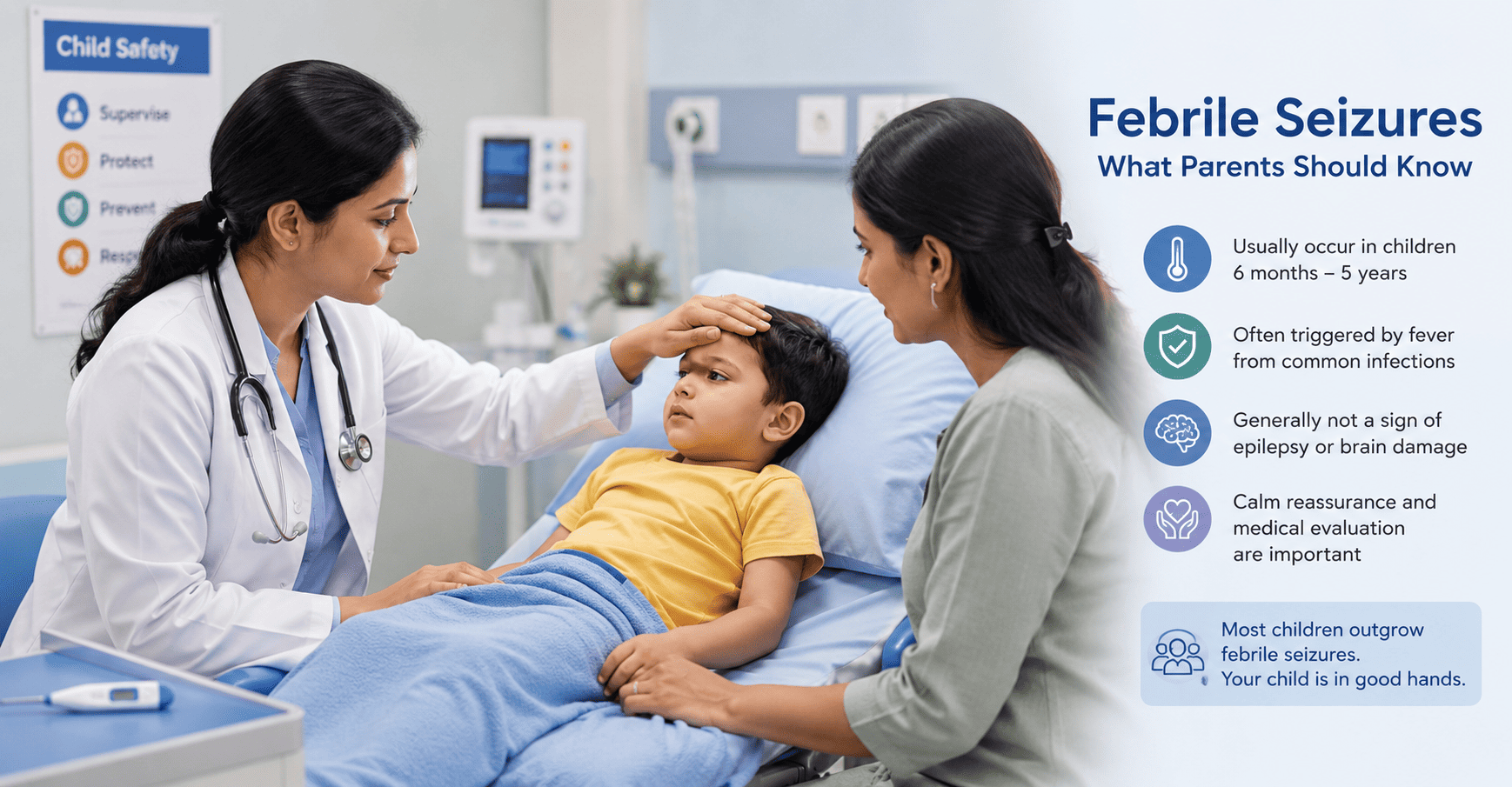
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
Febrile seizures remain one of the most frequently encountered neurological conditions in young children, particularly between 6 months and 5 years of age. They typically occur in association with fever during an acute illness without evidence of central nervous system infection or another clear intracranial cause. Because the event is often sudden and alarming, febrile seizures generate substantial parental anxiety and are a common reason for emergency consultation. From a clinical and scientific perspective, however, most febrile seizures are benign, brief, and not associated with long-term neurological injury when appropriately assessed.
Febrile seizures are generally classified into two main categories: simple febrile seizures and complex febrile seizures. A simple febrile seizure is generalized, lasts less than 15 minutes, and does not recur within 24 hours. In contrast, a complex febrile seizure may be prolonged, focal in onset or manifestation, or recur within the same febrile episode. This distinction is clinically important because it influences the need for further evaluation, follow-up strategy, and risk interpretation. Most febrile seizures are simple, and these cases usually carry an excellent prognosis.
The exact pathophysiology of febrile seizures is not fully understood, but age-dependent brain susceptibility appears to play a central role. The immature brain is believed to be more vulnerable to the effects of fever and inflammatory signaling. Genetic predisposition is also relevant, as children with a family history of febrile seizures or epilepsy may be at higher risk. Common triggers include viral upper respiratory tract infections, influenza, roseola, and other routine childhood febrile illnesses. In many cases, it may not be the absolute peak temperature alone, but the rapidity of temperature rise and the child’s neurobiological susceptibility that contribute to seizure occurrence.
The primary goal in evaluating a child with febrile seizure is not merely to confirm the seizure itself, but to identify the cause of fever and exclude serious conditions, especially meningitis or encephalitis. A thorough history should include seizure duration, semiology, recurrence, postictal behavior, recent illness, immunization status, developmental background, and prior neurological history. Physical examination should assess the child’s general condition, hydration, signs of focal infection, level of consciousness, meningeal signs, and focal neurological deficits. Clinical judgment is central, particularly in infants and in children whose presentation is not clearly consistent with a simple febrile seizure.
Current evidence-based guidelines do not support routine extensive neurodiagnostic testing in children with a clear simple febrile seizure who return to baseline and show no signs of central nervous system infection. Electroencephalography is not routinely indicated, and neuroimaging is generally unnecessary in uncomplicated cases. Lumbar puncture should be considered when meningitis is suspected, when the clinical examination is concerning, or in selected younger children with incomplete immunization status or atypical features. This selective approach helps avoid unnecessary procedures while preserving patient safety.
Acute management focuses first on supportive care. The child should be placed in a safe position, airway and breathing should be observed, and prolonged seizure activity should be managed promptly according to emergency protocols. Most febrile seizures stop spontaneously within a few minutes. If a seizure is prolonged, benzodiazepines may be required. After seizure cessation, attention should shift toward evaluation and management of the febrile illness. Antipyretics such as acetaminophen or ibuprofen may improve comfort, although they do not reliably prevent future febrile seizures.
One of the most important aspects of care is parental counseling. Families often fear brain damage, developmental impairment, or inevitable progression to epilepsy. In reality, the prognosis after a simple febrile seizure is generally very good. Most children recover fully and do not experience long-term cognitive or neurological consequences. Although recurrence can occur, especially in younger children or those with a family history, recurrent febrile seizures do not necessarily indicate chronic neurological disease. The risk of later epilepsy is slightly higher than in the general population, but remains low in most children with simple febrile seizures.
Long-term anticonvulsant prophylaxis is generally not recommended for simple febrile seizures because the adverse effects of chronic medication usually outweigh the benefits. Management should instead emphasize reassurance, education, and individualized guidance for future fever episodes. In selected cases involving prolonged seizures or recurrent complex episodes, emergency rescue medication strategies may be discussed with caregivers, but this should be based on careful clinical assessment rather than routine practice.
Overall, current scientific understanding supports a balanced view of febrile seizures in children. They are common, frightening to witness, and clinically important to evaluate, but they are usually benign. The key challenge is distinguishing low-risk febrile seizures from presentations that warrant further investigation. With careful assessment, appropriate supportive management, and clear communication with families, most children with febrile seizures can be managed safely and can be expected to have excellent long-term outcomes.
References
1. American Academy of Pediatrics, Subcommittee on Febrile Seizures. Febrile Seizures: Guideline for the Neurodiagnostic Evaluation of the Child With a Simple Febrile Seizure. Pediatrics. 2011.
2. American Academy of Pediatrics. Febrile Seizures: Clinical Practice Guideline for the Long-term Management of the Child With Simple Febrile Seizures. Pediatrics.
3. Patel N, Ram D, Swiderska N, et al. Febrile seizures. BMJ. 2015;351:h4240.
4. Leung AKC, Hon KL, Leung TNH. Febrile seizures: an overview. Drugs in Context. 2018;7:212536.
5. Berg AT, Shinnar S. Complex febrile seizures. Epilepsia. 1996;37(2):126-133.
Febrile seizures are generally classified into two main categories: simple febrile seizures and complex febrile seizures. A simple febrile seizure is generalized, lasts less than 15 minutes, and does not recur within 24 hours. In contrast, a complex febrile seizure may be prolonged, focal in onset or manifestation, or recur within the same febrile episode. This distinction is clinically important because it influences the need for further evaluation, follow-up strategy, and risk interpretation. Most febrile seizures are simple, and these cases usually carry an excellent prognosis.
The exact pathophysiology of febrile seizures is not fully understood, but age-dependent brain susceptibility appears to play a central role. The immature brain is believed to be more vulnerable to the effects of fever and inflammatory signaling. Genetic predisposition is also relevant, as children with a family history of febrile seizures or epilepsy may be at higher risk. Common triggers include viral upper respiratory tract infections, influenza, roseola, and other routine childhood febrile illnesses. In many cases, it may not be the absolute peak temperature alone, but the rapidity of temperature rise and the child’s neurobiological susceptibility that contribute to seizure occurrence.
The primary goal in evaluating a child with febrile seizure is not merely to confirm the seizure itself, but to identify the cause of fever and exclude serious conditions, especially meningitis or encephalitis. A thorough history should include seizure duration, semiology, recurrence, postictal behavior, recent illness, immunization status, developmental background, and prior neurological history. Physical examination should assess the child’s general condition, hydration, signs of focal infection, level of consciousness, meningeal signs, and focal neurological deficits. Clinical judgment is central, particularly in infants and in children whose presentation is not clearly consistent with a simple febrile seizure.
Current evidence-based guidelines do not support routine extensive neurodiagnostic testing in children with a clear simple febrile seizure who return to baseline and show no signs of central nervous system infection. Electroencephalography is not routinely indicated, and neuroimaging is generally unnecessary in uncomplicated cases. Lumbar puncture should be considered when meningitis is suspected, when the clinical examination is concerning, or in selected younger children with incomplete immunization status or atypical features. This selective approach helps avoid unnecessary procedures while preserving patient safety.
Acute management focuses first on supportive care. The child should be placed in a safe position, airway and breathing should be observed, and prolonged seizure activity should be managed promptly according to emergency protocols. Most febrile seizures stop spontaneously within a few minutes. If a seizure is prolonged, benzodiazepines may be required. After seizure cessation, attention should shift toward evaluation and management of the febrile illness. Antipyretics such as acetaminophen or ibuprofen may improve comfort, although they do not reliably prevent future febrile seizures.
One of the most important aspects of care is parental counseling. Families often fear brain damage, developmental impairment, or inevitable progression to epilepsy. In reality, the prognosis after a simple febrile seizure is generally very good. Most children recover fully and do not experience long-term cognitive or neurological consequences. Although recurrence can occur, especially in younger children or those with a family history, recurrent febrile seizures do not necessarily indicate chronic neurological disease. The risk of later epilepsy is slightly higher than in the general population, but remains low in most children with simple febrile seizures.
Long-term anticonvulsant prophylaxis is generally not recommended for simple febrile seizures because the adverse effects of chronic medication usually outweigh the benefits. Management should instead emphasize reassurance, education, and individualized guidance for future fever episodes. In selected cases involving prolonged seizures or recurrent complex episodes, emergency rescue medication strategies may be discussed with caregivers, but this should be based on careful clinical assessment rather than routine practice.
Overall, current scientific understanding supports a balanced view of febrile seizures in children. They are common, frightening to witness, and clinically important to evaluate, but they are usually benign. The key challenge is distinguishing low-risk febrile seizures from presentations that warrant further investigation. With careful assessment, appropriate supportive management, and clear communication with families, most children with febrile seizures can be managed safely and can be expected to have excellent long-term outcomes.
References
1. American Academy of Pediatrics, Subcommittee on Febrile Seizures. Febrile Seizures: Guideline for the Neurodiagnostic Evaluation of the Child With a Simple Febrile Seizure. Pediatrics. 2011.
2. American Academy of Pediatrics. Febrile Seizures: Clinical Practice Guideline for the Long-term Management of the Child With Simple Febrile Seizures. Pediatrics.
3. Patel N, Ram D, Swiderska N, et al. Febrile seizures. BMJ. 2015;351:h4240.
4. Leung AKC, Hon KL, Leung TNH. Febrile seizures: an overview. Drugs in Context. 2018;7:212536.
5. Berg AT, Shinnar S. Complex febrile seizures. Epilepsia. 1996;37(2):126-133.
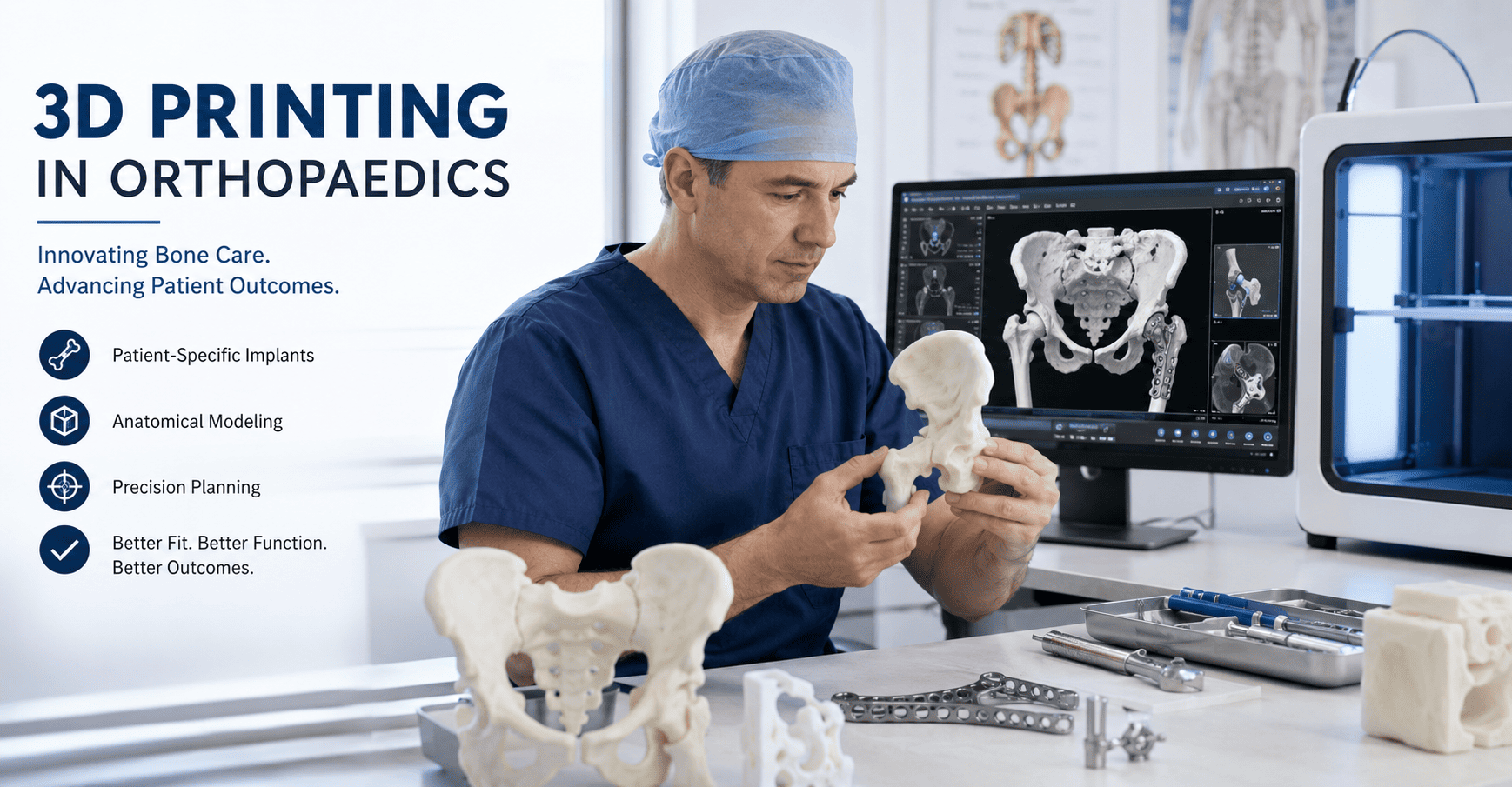
3D Printing in Orthopaedics: Expanding Precision, Personalization, and Surgical Planning in Modern Musculoskeletal Care
3D printing is increasingly reshaping orthopaedic practice by improving preoperative planning, implant customization, anatomical modeling, and educational simulation. Although challenges remain in cost, regulation, and standardization, the technology is becoming an important tool in precision musculoskeletal care.
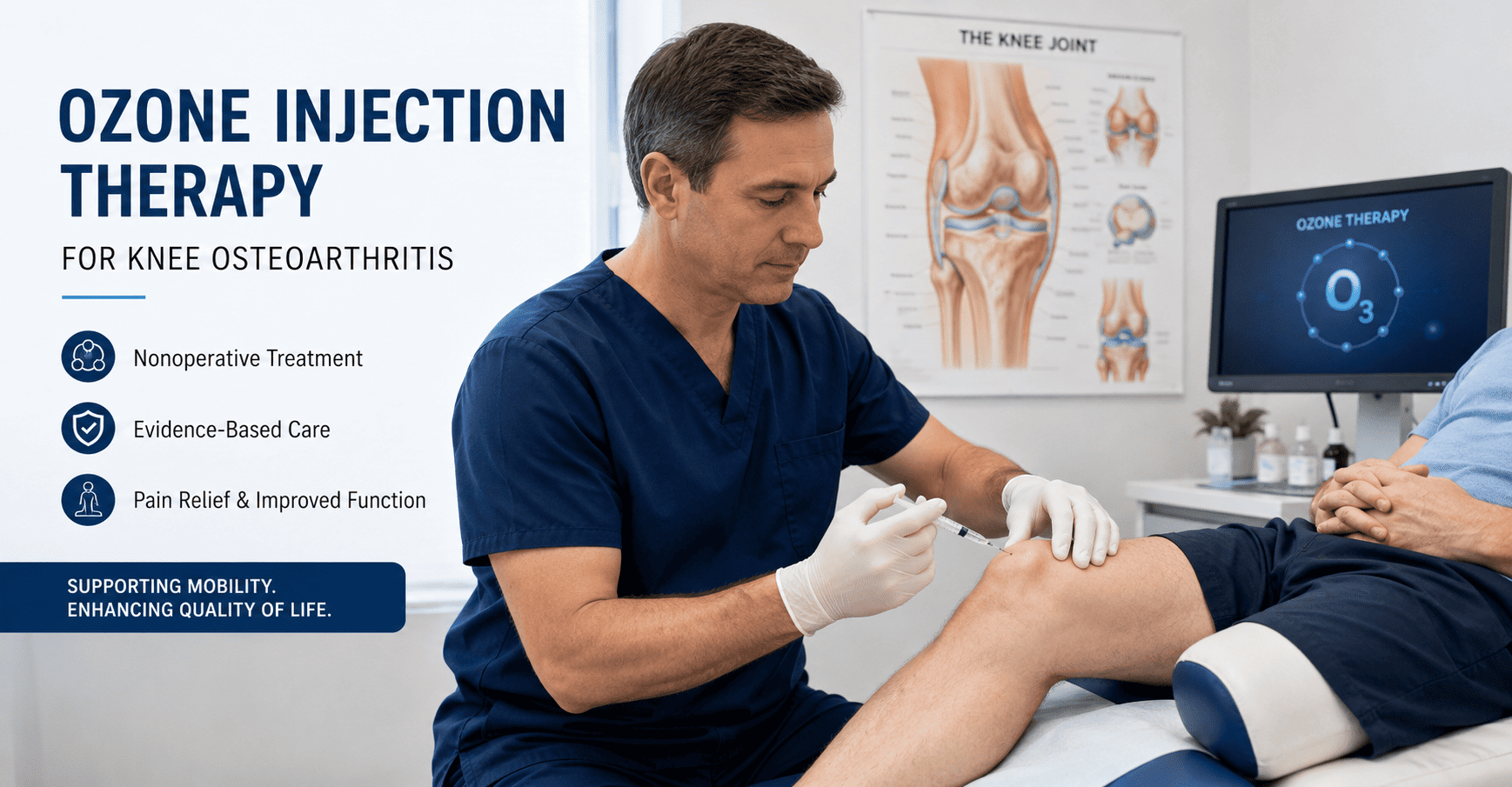
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps
Ozone injection therapy has gained attention as a nonoperative treatment option for knee osteoarthritis, particularly for short-term pain reduction and functional improvement. While early clinical findings are encouraging in selected patients, the therapy remains controversial because of inconsistent evidence quality, limited long-term data, and ongoing questions regarding standardization and comparative effectiveness.
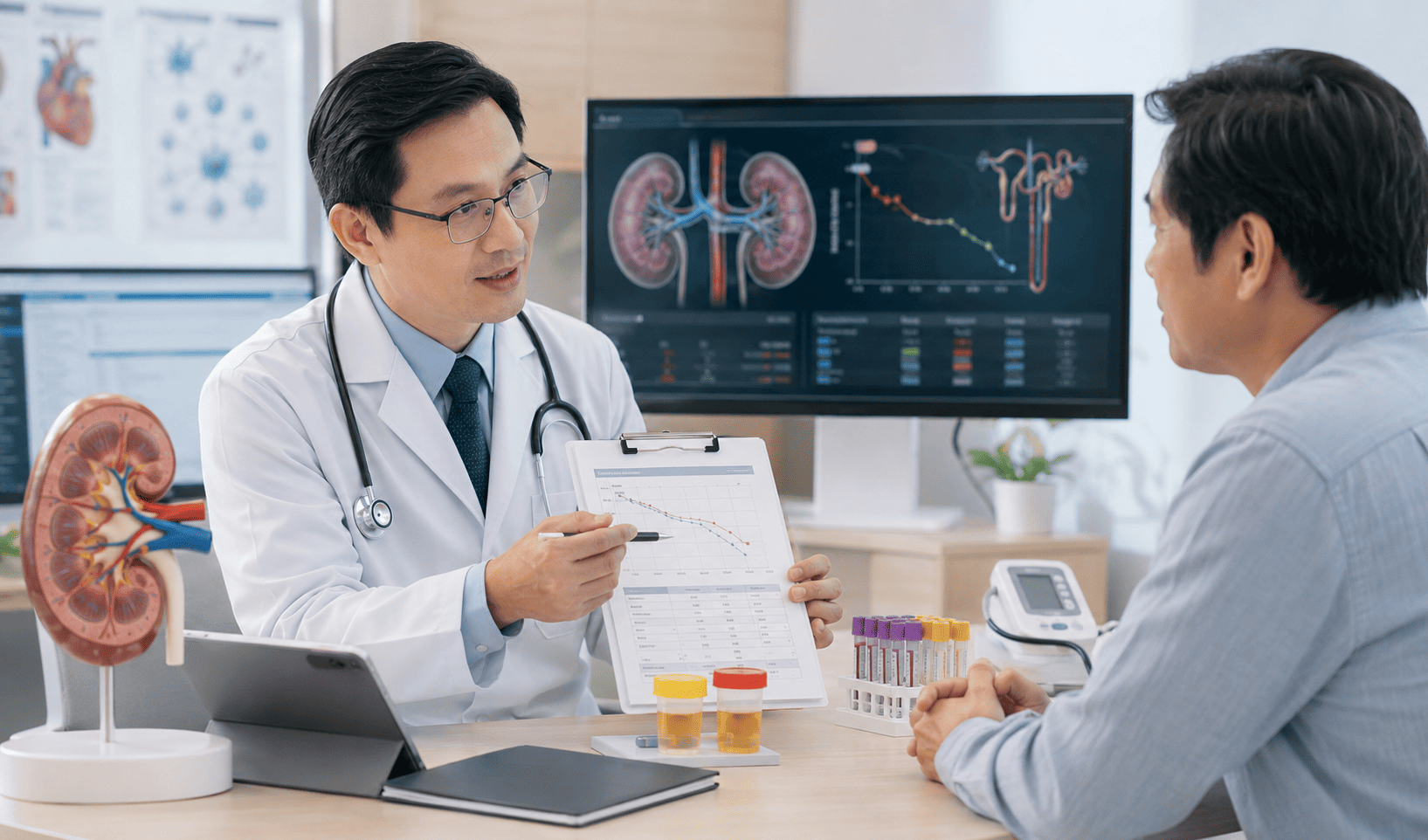
Chronic Kidney Disease: Early Detection and Risk Control Remain Central to Better Outcomes
Chronic kidney disease (CKD) continues to pose a major global health challenge due to its high prevalence, silent progression, and close association with cardiovascular complications. Early screening, timely diagnosis, and better control of diabetes and hypertension remain essential to slow disease progression and reduce kidney failure and mortality.
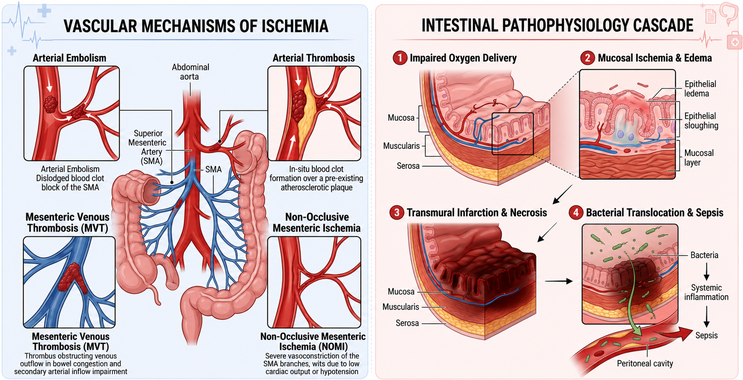
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.