-
-
-
Jakarta, Indonesia
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps
Knee osteoarthritis remains a major cause of chronic pain, impaired mobility, and reduced quality of life worldwide. As the condition progresses, patients commonly experience joint stiffness, activity-related pain, crepitus, and functional limitation that gradually interfere with daily living. Standard nonoperative management continues to include exercise therapy, weight reduction, physical rehabilitation, analgesics, topical agents, and selected intra-articular interventions before surgical treatment is considered. Within this therapeutic landscape, ozone injection therapy has emerged as a proposed minimally invasive option for symptom control in carefully selected patients.
Medical ozone is typically administered as an oxygen-ozone gas mixture through intra-articular injection. Its proposed mechanism is not based on structural cartilage regeneration alone, but rather on modulation of inflammation, oxidative stress signaling, and nociceptive pathways. Some investigators suggest that controlled ozone exposure may induce a biochemical response that improves the intra-articular environment, reduces inflammatory mediators, and contributes to pain relief. This theoretical rationale has supported broader interest in ozone treatment, especially in patients seeking alternatives to corticosteroids, repeated oral analgesics, or early surgery.
From a clinical perspective, the main attraction of ozone therapy lies in its relative simplicity and outpatient feasibility. It is generally described as a low-cost procedure, does not require major instrumentation, and has been explored in a range of musculoskeletal pain disorders. In knee osteoarthritis specifically, several studies have reported improvement in pain scores and joint function after serial injections. These findings have encouraged use in some rehabilitation, sports medicine, and pain management settings. However, the interpretation of such results requires caution because trial methodology, dose protocols, and comparator selection vary substantially across studies.
A key issue in the scientific discussion is heterogeneity. Published studies differ in ozone concentration, injection volume, treatment frequency, patient severity, outcome measurement, and follow-up duration. Some trials compare ozone with hyaluronic acid, some with placebo, and others with exercise-based care or standard conservative treatment. This inconsistency makes it difficult to define where ozone therapy truly fits within evidence-based osteoarthritis care. In addition, many available studies involve modest sample sizes and relatively short observation periods, which limits confidence in long-term benefit.
Current evidence suggests that ozone injection may provide short-term symptomatic improvement in some patients, especially in pain reduction and functional scores. Yet the degree of benefit relative to established intra-articular treatments remains uncertain. Corticosteroid injections may offer rapid anti-inflammatory relief, while hyaluronic acid is still used selectively in certain settings despite ongoing debate about magnitude of effect. Ozone therapy is therefore not yet positioned as a universal replacement for standard injections. Instead, it is better understood as a possible adjunctive option that may be considered where appropriate expertise, patient counseling, and clinical selection are available.
Patient selection is especially important. Ozone therapy may be more reasonably discussed in individuals with mild to moderate symptomatic knee osteoarthritis who remain limited despite conservative management but are not yet candidates for arthroplasty or do not wish to proceed with surgery. It may also be considered in settings where repeated corticosteroid exposure is undesirable. At the same time, severe structural degeneration, marked malalignment, advanced inflammatory joint disease, or unrealistic expectations may reduce the likelihood of meaningful benefit. As with many injection-based therapies in osteoarthritis, success depends not only on the substance injected but also on the broader treatment strategy, including rehabilitation, strengthening, weight control, and biomechanical support.
Safety data reported so far are generally reassuring when the procedure is performed correctly under appropriate sterile technique. Most adverse effects described are mild and transient, such as localized discomfort or temporary post-injection pain. Nevertheless, safety should not be assumed uncritically. Standardization of preparation, concentration, procedural technique, and practitioner training remains essential. Any intra-articular procedure carries potential procedural risks, and the absence of major complications in smaller studies does not eliminate the need for careful monitoring in wider use.
Another important consideration is how ozone therapy is communicated to patients. Because it is sometimes presented in promotional language as a regenerative or highly innovative treatment, there is a risk of overstating the certainty of benefit. For scientific and ethical reasons, patients should be informed that ozone injection therapy remains an evolving modality rather than an unequivocally established standard of care. Shared decision-making should include discussion of expected symptom relief, evidence limitations, alternative nonsurgical options, cost considerations, and the likely need for combined lifestyle and rehabilitation measures.
From an orthopaedic and musculoskeletal medicine perspective, ozone injection therapy reflects a broader shift toward less invasive symptom-targeted interventions for degenerative joint disease. This trend is understandable, especially as patients increasingly seek treatments that may postpone surgery while preserving function. Still, enthusiasm should be balanced by clinical discipline. Better-designed randomized trials, longer follow-up, clearer procedural standardization, and stronger head-to-head comparisons with accepted therapies are needed before ozone injection can be more confidently integrated into mainstream treatment algorithms.
In summary, ozone injection therapy for knee osteoarthritis remains a promising but incompletely defined intervention. It may offer symptomatic benefit in selected patients, particularly for short-term pain and function, but current evidence does not fully resolve its long-term role or comparative value. Until stronger data become available, ozone therapy should be approached as a selective adjunct within individualized osteoarthritis care rather than as a definitive solution for all patients with knee degeneration.
References
1. Raeissadat SA, Rayegani SM, Hasanabadi H, et al. Knee Osteoarthritis Injection Choices: Platelet-Rich Plasma, Hyaluronic Acid, or Ozone Therapy? A Randomized Clinical Trial. Pain Research and Management. 2018.
2. Sconza C, Respizzi S, Virelli L, et al. Oxygen-Ozone Therapy for the Treatment of Knee Osteoarthritis: A Systematic Review of Randomized Controlled Trials. Cartilage.
3. Babaei-Ghazani A, Najarzadeh A, Mansoori K, et al. Ozone Therapy in Knee Osteoarthritis: A Systematic Review and Meta-analysis. PM&R.
4. Bannuru RR, Osani MC, Vaysbrot EE, et al. OARSI Guidelines for the Non-Surgical Management of Knee, Hip, and Polyarticular Osteoarthritis. Osteoarthritis and Cartilage. 2019.
5. Kolasinski SL, Neogi T, Hochberg MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care & Research. 2020.
Medical ozone is typically administered as an oxygen-ozone gas mixture through intra-articular injection. Its proposed mechanism is not based on structural cartilage regeneration alone, but rather on modulation of inflammation, oxidative stress signaling, and nociceptive pathways. Some investigators suggest that controlled ozone exposure may induce a biochemical response that improves the intra-articular environment, reduces inflammatory mediators, and contributes to pain relief. This theoretical rationale has supported broader interest in ozone treatment, especially in patients seeking alternatives to corticosteroids, repeated oral analgesics, or early surgery.
From a clinical perspective, the main attraction of ozone therapy lies in its relative simplicity and outpatient feasibility. It is generally described as a low-cost procedure, does not require major instrumentation, and has been explored in a range of musculoskeletal pain disorders. In knee osteoarthritis specifically, several studies have reported improvement in pain scores and joint function after serial injections. These findings have encouraged use in some rehabilitation, sports medicine, and pain management settings. However, the interpretation of such results requires caution because trial methodology, dose protocols, and comparator selection vary substantially across studies.
A key issue in the scientific discussion is heterogeneity. Published studies differ in ozone concentration, injection volume, treatment frequency, patient severity, outcome measurement, and follow-up duration. Some trials compare ozone with hyaluronic acid, some with placebo, and others with exercise-based care or standard conservative treatment. This inconsistency makes it difficult to define where ozone therapy truly fits within evidence-based osteoarthritis care. In addition, many available studies involve modest sample sizes and relatively short observation periods, which limits confidence in long-term benefit.
Current evidence suggests that ozone injection may provide short-term symptomatic improvement in some patients, especially in pain reduction and functional scores. Yet the degree of benefit relative to established intra-articular treatments remains uncertain. Corticosteroid injections may offer rapid anti-inflammatory relief, while hyaluronic acid is still used selectively in certain settings despite ongoing debate about magnitude of effect. Ozone therapy is therefore not yet positioned as a universal replacement for standard injections. Instead, it is better understood as a possible adjunctive option that may be considered where appropriate expertise, patient counseling, and clinical selection are available.
Patient selection is especially important. Ozone therapy may be more reasonably discussed in individuals with mild to moderate symptomatic knee osteoarthritis who remain limited despite conservative management but are not yet candidates for arthroplasty or do not wish to proceed with surgery. It may also be considered in settings where repeated corticosteroid exposure is undesirable. At the same time, severe structural degeneration, marked malalignment, advanced inflammatory joint disease, or unrealistic expectations may reduce the likelihood of meaningful benefit. As with many injection-based therapies in osteoarthritis, success depends not only on the substance injected but also on the broader treatment strategy, including rehabilitation, strengthening, weight control, and biomechanical support.
Safety data reported so far are generally reassuring when the procedure is performed correctly under appropriate sterile technique. Most adverse effects described are mild and transient, such as localized discomfort or temporary post-injection pain. Nevertheless, safety should not be assumed uncritically. Standardization of preparation, concentration, procedural technique, and practitioner training remains essential. Any intra-articular procedure carries potential procedural risks, and the absence of major complications in smaller studies does not eliminate the need for careful monitoring in wider use.
Another important consideration is how ozone therapy is communicated to patients. Because it is sometimes presented in promotional language as a regenerative or highly innovative treatment, there is a risk of overstating the certainty of benefit. For scientific and ethical reasons, patients should be informed that ozone injection therapy remains an evolving modality rather than an unequivocally established standard of care. Shared decision-making should include discussion of expected symptom relief, evidence limitations, alternative nonsurgical options, cost considerations, and the likely need for combined lifestyle and rehabilitation measures.
From an orthopaedic and musculoskeletal medicine perspective, ozone injection therapy reflects a broader shift toward less invasive symptom-targeted interventions for degenerative joint disease. This trend is understandable, especially as patients increasingly seek treatments that may postpone surgery while preserving function. Still, enthusiasm should be balanced by clinical discipline. Better-designed randomized trials, longer follow-up, clearer procedural standardization, and stronger head-to-head comparisons with accepted therapies are needed before ozone injection can be more confidently integrated into mainstream treatment algorithms.
In summary, ozone injection therapy for knee osteoarthritis remains a promising but incompletely defined intervention. It may offer symptomatic benefit in selected patients, particularly for short-term pain and function, but current evidence does not fully resolve its long-term role or comparative value. Until stronger data become available, ozone therapy should be approached as a selective adjunct within individualized osteoarthritis care rather than as a definitive solution for all patients with knee degeneration.
References
1. Raeissadat SA, Rayegani SM, Hasanabadi H, et al. Knee Osteoarthritis Injection Choices: Platelet-Rich Plasma, Hyaluronic Acid, or Ozone Therapy? A Randomized Clinical Trial. Pain Research and Management. 2018.
2. Sconza C, Respizzi S, Virelli L, et al. Oxygen-Ozone Therapy for the Treatment of Knee Osteoarthritis: A Systematic Review of Randomized Controlled Trials. Cartilage.
3. Babaei-Ghazani A, Najarzadeh A, Mansoori K, et al. Ozone Therapy in Knee Osteoarthritis: A Systematic Review and Meta-analysis. PM&R.
4. Bannuru RR, Osani MC, Vaysbrot EE, et al. OARSI Guidelines for the Non-Surgical Management of Knee, Hip, and Polyarticular Osteoarthritis. Osteoarthritis and Cartilage. 2019.
5. Kolasinski SL, Neogi T, Hochberg MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care & Research. 2020.
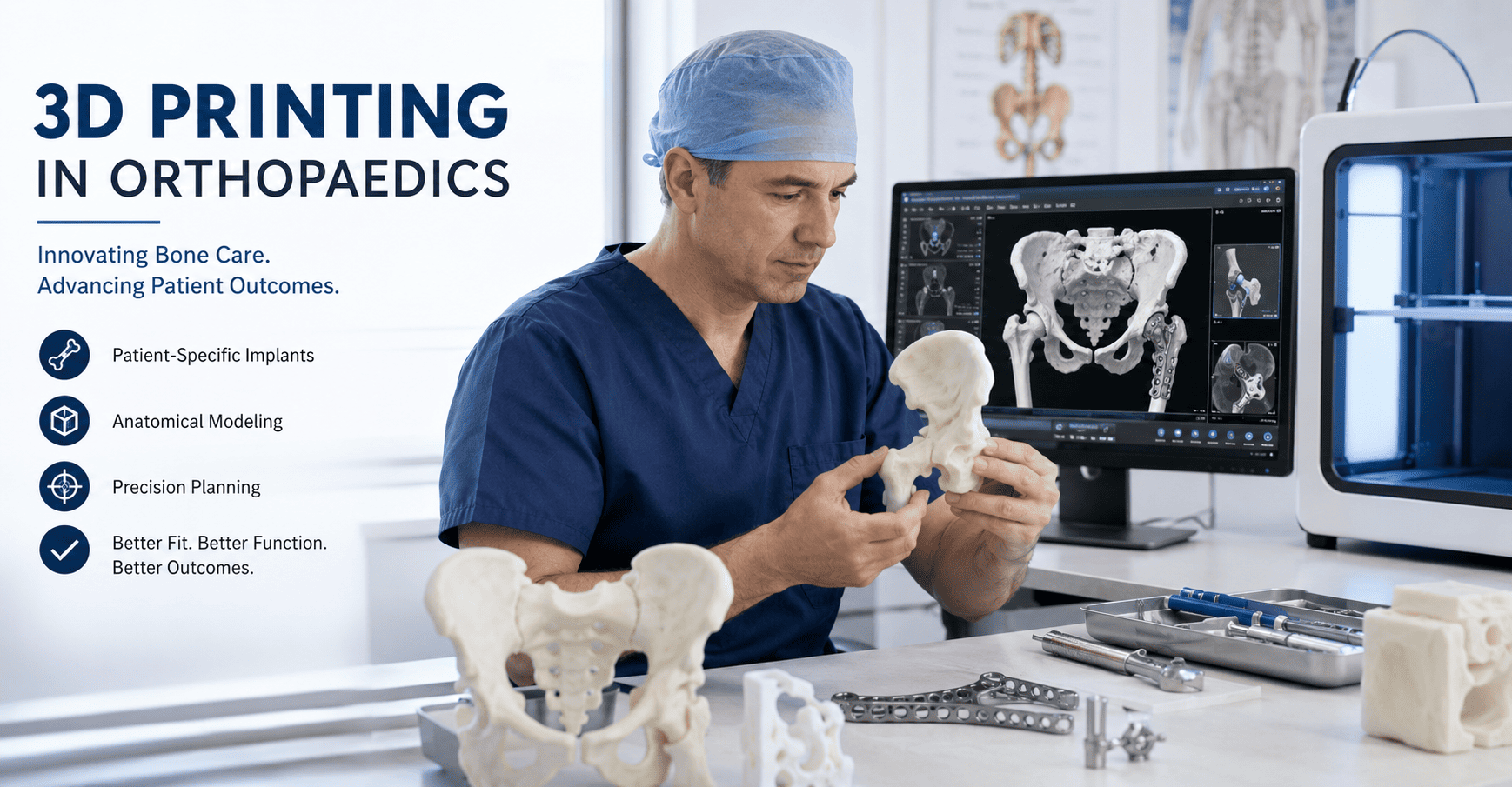
3D Printing in Orthopaedics: Expanding Precision, Personalization, and Surgical Planning in Modern Musculoskeletal Care
3D printing is increasingly reshaping orthopaedic practice by improving preoperative planning, implant customization, anatomical modeling, and educational simulation. Although challenges remain in cost, regulation, and standardization, the technology is becoming an important tool in precision musculoskeletal care.
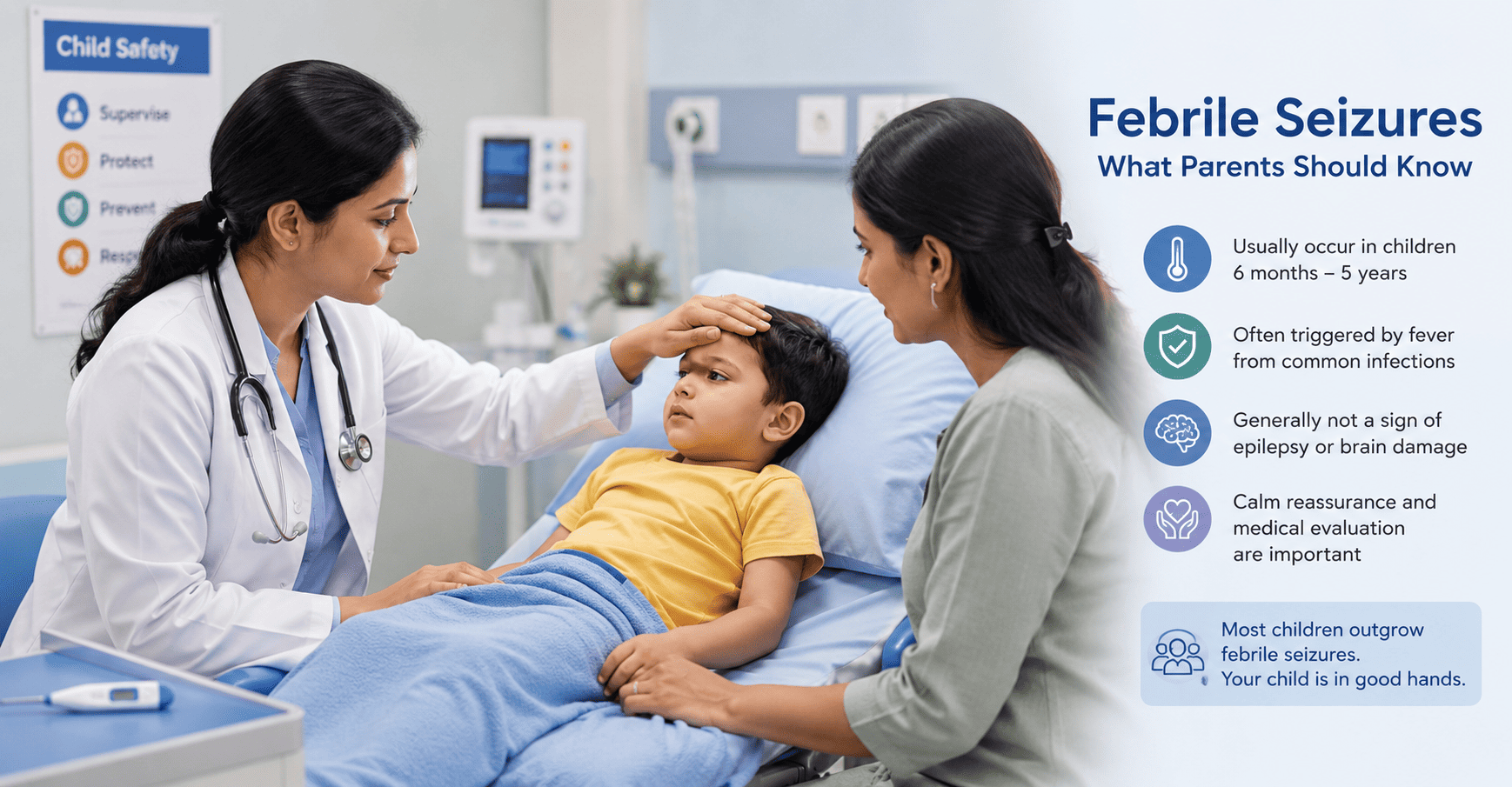
Febrile Seizures in Children: Common and Usually Benign, but Accurate Clinical Assessment Remains Essential
Febrile seizures are among the most common neurological events in early childhood and are generally associated with a favorable prognosis. Although most cases are simple and self-limited, careful clinical evaluation remains important to distinguish benign febrile seizures from central nervous system infection, epilepsy, or other serious underlying conditions.
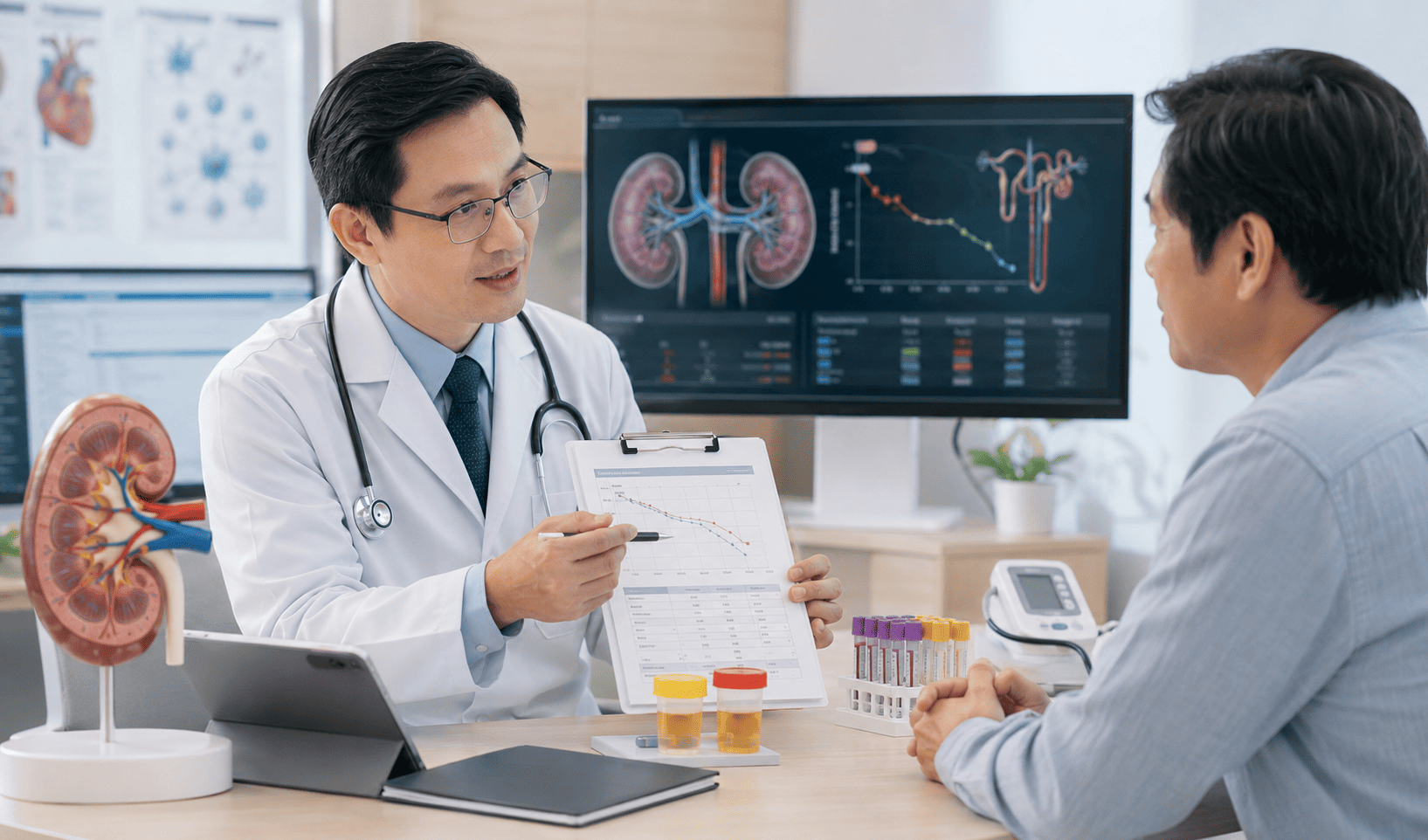
Chronic Kidney Disease: Early Detection and Risk Control Remain Central to Better Outcomes
Chronic kidney disease (CKD) continues to pose a major global health challenge due to its high prevalence, silent progression, and close association with cardiovascular complications. Early screening, timely diagnosis, and better control of diabetes and hypertension remain essential to slow disease progression and reduce kidney failure and mortality.
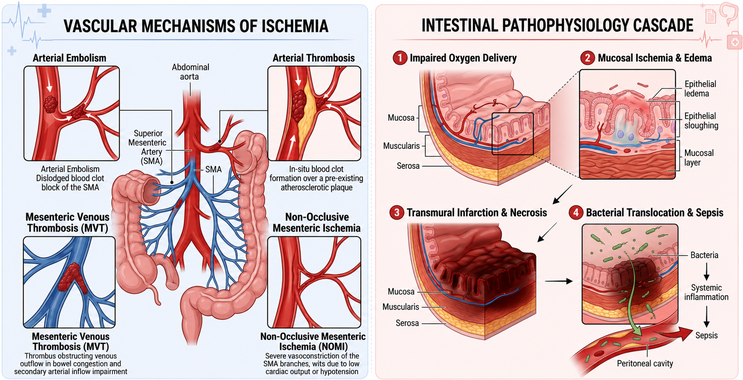
Acute Mesenteric Ischemia: A Vascular Emergency That Requires Immediate Recognition
Acute mesenteric ischemia is a life-threatening vascular emergency caused by a sudden reduction in intestinal blood flow. Because its early symptoms may appear nonspecific, delayed diagnosis remains common and is strongly associated with bowel necrosis, sepsis, and high mortality.