-
-
-
Jakarta, Indonesia
Blood Pressure Monitoring as a Public Health Priority: Strengthening Early Detection and Long-Term Cardiovascular Prevention

Understanding Stunted Children: Chronic Growth Failure, Early-Life Risks, and Why It Matters Beyond Height
Stunting remains one of the most important indicators of chronic child undernutrition and early-life vulnerability worldwide. In pediatric and public health practice, the term refers to a child who is too short for age as a result of long-term growth restriction rather than normal genetic variation alone. According to international growth standards, a child is considered stunted when height-for-age is more than two standard deviations below the median of the World Health Organization child growth reference. This definition provides a measurable clinical threshold, but the broader meaning of stunting extends far beyond anthropometric classification.
At its core, stunting reflects prolonged failure to achieve expected linear growth during critical periods of development, especially from pregnancy through the first two years of life. This period, often described as the first 1,000 days, is biologically sensitive because nutrition, infection burden, maternal health, and caregiving conditions interact intensively to shape growth and organ development. When these early influences are persistently unfavorable, the child may not simply become shorter than peers, but may also experience wider developmental consequences that affect health across the life course.
A common misunderstanding is to view stunting as merely a body size issue. In reality, it is best understood as a marker of chronic adversity affecting multiple systems. Children who are stunted may face increased vulnerability in cognitive development, learning capacity, immune resilience, and later productivity. The condition is therefore not only a pediatric growth concern, but also a signal of deeper nutritional, infectious, environmental, and socioeconomic inequality. This is why stunting is widely used in global child health as both a clinical and developmental indicator.
The causes of stunting are multifactorial and cumulative. Chronic inadequate nutrient intake remains central, particularly deficiencies in energy, protein, and essential micronutrients such as iron, zinc, iodine, and vitamin A. However, food intake alone does not explain the entire problem. Recurrent infections, especially diarrhea, respiratory illness, intestinal parasitic disease, and poor sanitation, can repeatedly impair nutrient absorption and increase metabolic stress. Maternal malnutrition, low birth weight, suboptimal breastfeeding, delayed or poor-quality complementary feeding, and household poverty further contribute to the risk. In this way, stunting develops through repeated biological disadvantage rather than from a single event.
Prenatal influences are especially important in understanding stunting. Poor maternal nutrition before and during pregnancy can affect fetal growth and set the stage for postnatal growth failure. Mothers with anemia, inadequate caloric intake, adolescent pregnancy, or limited access to antenatal care may be more likely to deliver infants already at nutritional disadvantage. Thus, the concept of a stunted child often begins before birth. By the time poor growth becomes clearly visible in early childhood, the underlying process may already have been present for many months.
Clinically, not every short child is stunted, and not every child with growth concern has malnutrition as the primary explanation. Some children are constitutionally small or come from families with shorter genetic stature. Others may have endocrine disorders, chronic systemic disease, congenital syndromes, or gastrointestinal conditions affecting growth. For this reason, accurate assessment is essential. Pediatric evaluation should include serial growth measurement, review of dietary history, infection history, developmental milestones, birth history, family growth patterns, and social context. The diagnosis of stunting should be made thoughtfully and ideally supported by proper growth chart interpretation rather than casual visual judgment.
The consequences of stunting can be long-lasting. Studies have linked chronic early growth restriction with poorer cognitive performance, delayed school achievement, and reduced adult earning potential. Stunting has also been associated with altered metabolic programming, raising concern that some individuals may face increased risk of obesity, diabetes, or cardiovascular disease later in life when exposed to unhealthy nutritional transitions. These long-term effects make stunting more than a pediatric nutrition diagnosis; it is a condition with lifelong developmental and societal implications.
Prevention of stunting requires a comprehensive approach rather than isolated feeding advice. Maternal nutrition, quality antenatal care, exclusive breastfeeding, timely and nutrient-rich complementary feeding, immunization, infection prevention, sanitation, and family education all play important roles. In many communities, the strongest gains come from integrated interventions that combine health services with clean water access, poverty reduction, and nutrition-sensitive social support. Because the causes are layered, the response must also be layered.
From a pediatric communication perspective, explaining the meaning of stunting to families requires care and clarity. The term should not be used in a stigmatizing way or reduced to a label of failure. Instead, it should help families understand that child growth reflects overall health conditions over time. Early identification is valuable because the earlier a growth problem is recognized, the greater the opportunity for nutritional correction, developmental support, and prevention of further decline. Delayed recognition limits the chance for catch-up growth and broader developmental recovery.
In summary, a stunted child is not simply a child who is shorter than average, but a child whose linear growth has been chronically restricted by adverse biological and environmental influences. The concept of stunting captures the cumulative effects of undernutrition, recurrent infection, and early-life disadvantage during critical developmental windows. Understanding stunting in this fuller sense is essential for pediatric care, family counseling, and public health planning, because the issue concerns not only stature, but also the future health and developmental potential of the child.
References
1. World Health Organization. WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age. WHO.
2. de Onis M, Branca F. Childhood stunting: a global perspective. Maternal and Child Nutrition. 2016;12(Suppl 1):12-26.
3. Black RE, Victora CG, Walker SP, et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. The Lancet. 2013;382(9890):427-451.
4. Stewart CP, Iannotti L, Dewey KG, Michaelsen KF, Onyango AW. Contextualizing complementary feeding in a broader framework for stunting prevention. Maternal and Child Nutrition. 2013;9(Suppl 2):27-45.
5. Victora CG, Adair L, Fall C, et al. Maternal and child undernutrition: consequences for adult health and human capital. The Lancet. 2008;371(9609):340-357.
At its core, stunting reflects prolonged failure to achieve expected linear growth during critical periods of development, especially from pregnancy through the first two years of life. This period, often described as the first 1,000 days, is biologically sensitive because nutrition, infection burden, maternal health, and caregiving conditions interact intensively to shape growth and organ development. When these early influences are persistently unfavorable, the child may not simply become shorter than peers, but may also experience wider developmental consequences that affect health across the life course.
A common misunderstanding is to view stunting as merely a body size issue. In reality, it is best understood as a marker of chronic adversity affecting multiple systems. Children who are stunted may face increased vulnerability in cognitive development, learning capacity, immune resilience, and later productivity. The condition is therefore not only a pediatric growth concern, but also a signal of deeper nutritional, infectious, environmental, and socioeconomic inequality. This is why stunting is widely used in global child health as both a clinical and developmental indicator.
The causes of stunting are multifactorial and cumulative. Chronic inadequate nutrient intake remains central, particularly deficiencies in energy, protein, and essential micronutrients such as iron, zinc, iodine, and vitamin A. However, food intake alone does not explain the entire problem. Recurrent infections, especially diarrhea, respiratory illness, intestinal parasitic disease, and poor sanitation, can repeatedly impair nutrient absorption and increase metabolic stress. Maternal malnutrition, low birth weight, suboptimal breastfeeding, delayed or poor-quality complementary feeding, and household poverty further contribute to the risk. In this way, stunting develops through repeated biological disadvantage rather than from a single event.
Prenatal influences are especially important in understanding stunting. Poor maternal nutrition before and during pregnancy can affect fetal growth and set the stage for postnatal growth failure. Mothers with anemia, inadequate caloric intake, adolescent pregnancy, or limited access to antenatal care may be more likely to deliver infants already at nutritional disadvantage. Thus, the concept of a stunted child often begins before birth. By the time poor growth becomes clearly visible in early childhood, the underlying process may already have been present for many months.
Clinically, not every short child is stunted, and not every child with growth concern has malnutrition as the primary explanation. Some children are constitutionally small or come from families with shorter genetic stature. Others may have endocrine disorders, chronic systemic disease, congenital syndromes, or gastrointestinal conditions affecting growth. For this reason, accurate assessment is essential. Pediatric evaluation should include serial growth measurement, review of dietary history, infection history, developmental milestones, birth history, family growth patterns, and social context. The diagnosis of stunting should be made thoughtfully and ideally supported by proper growth chart interpretation rather than casual visual judgment.
The consequences of stunting can be long-lasting. Studies have linked chronic early growth restriction with poorer cognitive performance, delayed school achievement, and reduced adult earning potential. Stunting has also been associated with altered metabolic programming, raising concern that some individuals may face increased risk of obesity, diabetes, or cardiovascular disease later in life when exposed to unhealthy nutritional transitions. These long-term effects make stunting more than a pediatric nutrition diagnosis; it is a condition with lifelong developmental and societal implications.
Prevention of stunting requires a comprehensive approach rather than isolated feeding advice. Maternal nutrition, quality antenatal care, exclusive breastfeeding, timely and nutrient-rich complementary feeding, immunization, infection prevention, sanitation, and family education all play important roles. In many communities, the strongest gains come from integrated interventions that combine health services with clean water access, poverty reduction, and nutrition-sensitive social support. Because the causes are layered, the response must also be layered.
From a pediatric communication perspective, explaining the meaning of stunting to families requires care and clarity. The term should not be used in a stigmatizing way or reduced to a label of failure. Instead, it should help families understand that child growth reflects overall health conditions over time. Early identification is valuable because the earlier a growth problem is recognized, the greater the opportunity for nutritional correction, developmental support, and prevention of further decline. Delayed recognition limits the chance for catch-up growth and broader developmental recovery.
In summary, a stunted child is not simply a child who is shorter than average, but a child whose linear growth has been chronically restricted by adverse biological and environmental influences. The concept of stunting captures the cumulative effects of undernutrition, recurrent infection, and early-life disadvantage during critical developmental windows. Understanding stunting in this fuller sense is essential for pediatric care, family counseling, and public health planning, because the issue concerns not only stature, but also the future health and developmental potential of the child.
References
1. World Health Organization. WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age. WHO.
2. de Onis M, Branca F. Childhood stunting: a global perspective. Maternal and Child Nutrition. 2016;12(Suppl 1):12-26.
3. Black RE, Victora CG, Walker SP, et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. The Lancet. 2013;382(9890):427-451.
4. Stewart CP, Iannotti L, Dewey KG, Michaelsen KF, Onyango AW. Contextualizing complementary feeding in a broader framework for stunting prevention. Maternal and Child Nutrition. 2013;9(Suppl 2):27-45.
5. Victora CG, Adair L, Fall C, et al. Maternal and child undernutrition: consequences for adult health and human capital. The Lancet. 2008;371(9609):340-357.
Papaya Consumption and Health Benefits: Nutritional Value, Digestive Support, and Its Role in a Balanced Diet
Papaya is a nutrient-dense tropical fruit that offers a range of health benefits, particularly through its vitamin content, fiber, antioxidant compounds, and digestive enzyme activity. Regular papaya consumption may support gastrointestinal health, immune function, and overall dietary quality when included as part of a balanced nutritional pattern.
Blood Pressure Monitoring as a Public Health Priority: Strengthening Early Detection and Long-Term Cardiovascular Prevention
Blood pressure monitoring remains one of the most practical and impactful tools in public health for identifying hypertension early, guiding treatment decisions, and reducing long-term cardiovascular risk. Wider adoption of accurate office, community, and home-based monitoring strategies could significantly improve prevention of stroke, heart disease, kidney damage, and premature mortality.
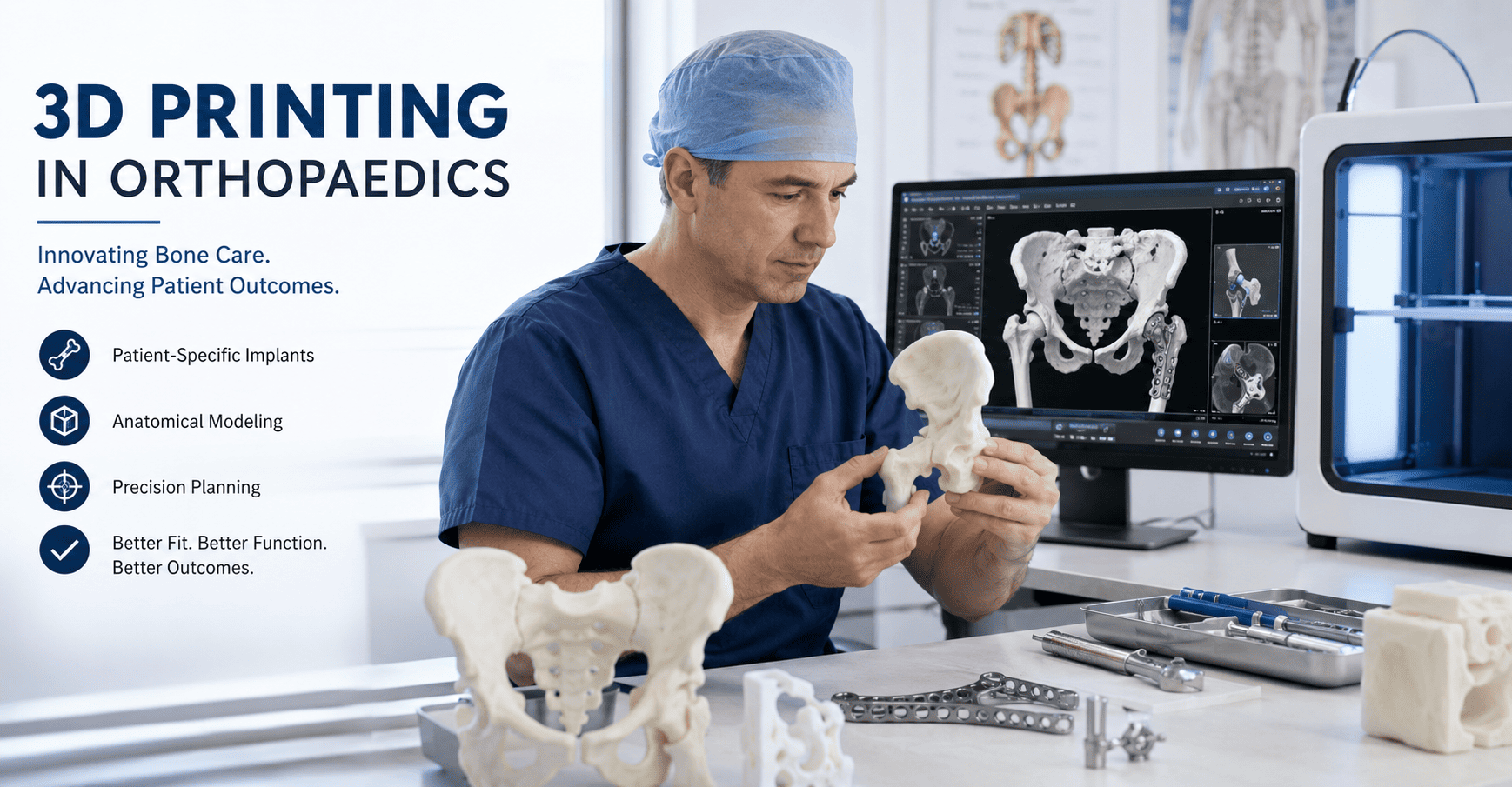
3D Printing in Orthopaedics: Expanding Precision, Personalization, and Surgical Planning in Modern Musculoskeletal Care
3D printing is increasingly reshaping orthopaedic practice by improving preoperative planning, implant customization, anatomical modeling, and educational simulation. Although challenges remain in cost, regulation, and standardization, the technology is becoming an important tool in precision musculoskeletal care.
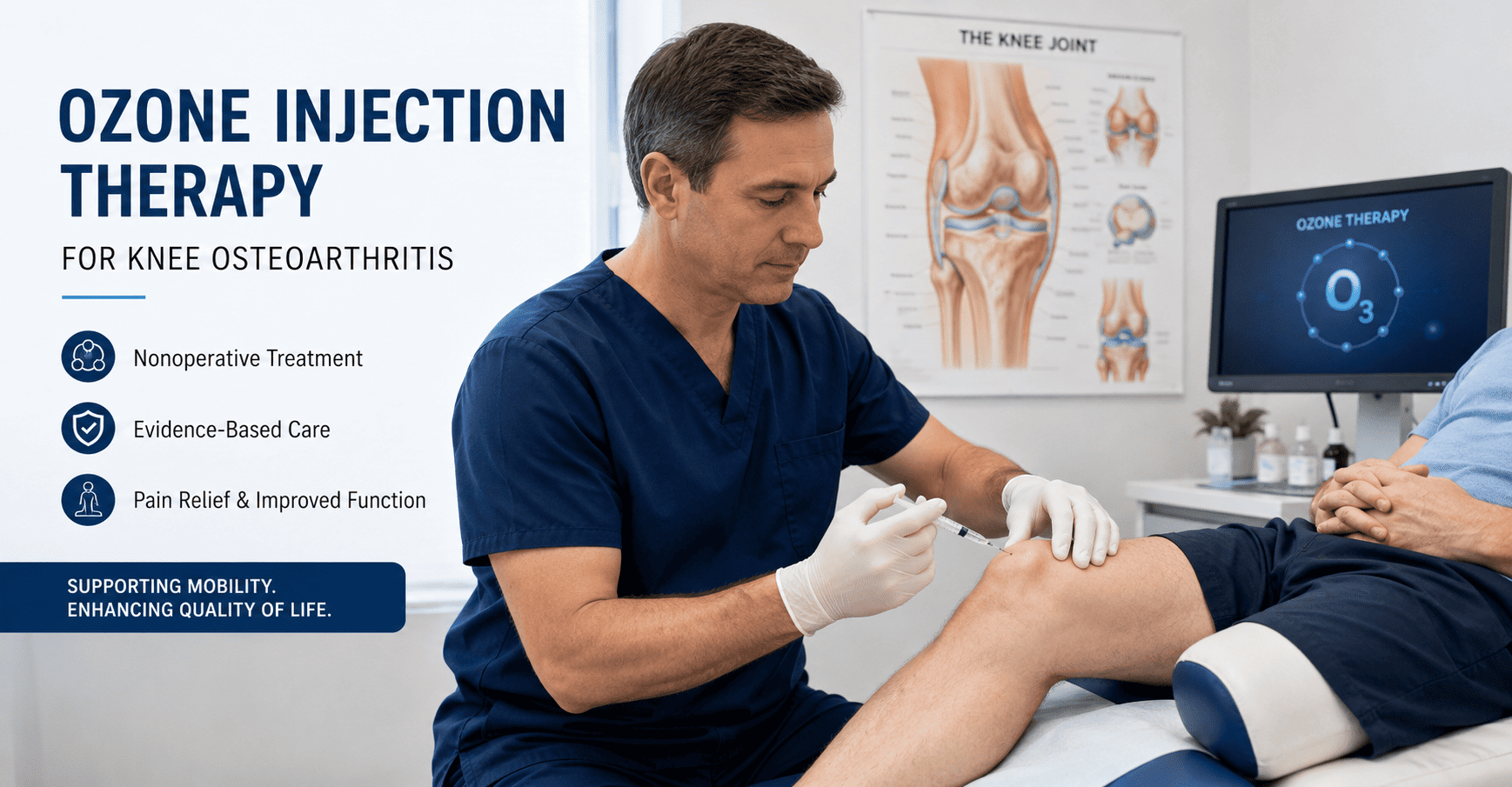
Ozone Injection Therapy in Knee Osteoarthritis: Emerging Adjunctive Option Amid Ongoing Evidence Gaps
Ozone injection therapy has gained attention as a nonoperative treatment option for knee osteoarthritis, particularly for short-term pain reduction and functional improvement. While early clinical findings are encouraging in selected patients, the therapy remains controversial because of inconsistent evidence quality, limited long-term data, and ongoing questions regarding standardization and comparative effectiveness.